- Author: Kathy Keatley Garvey

A natural product from the dried root of a pea-family plant, potentially combined with an enzyme inhibitor discovered in the Bruce Hammock laboratory at the University of California, Davis, may provide hope in alleviating neuroinflammation in Parkinson's disease, an eight-member team of researchers from Dalian Medical University, China, and UC Davis announced today.
Their novel research, published in the current edition of the Proceedings of the National Academy of Sciences (PNAS), shows that a soluble epoxide hydrolase (sEH) inhibitor and kurarinone, a compound from the dried root of Sophora flavescens, reduced neuroinflammation in an animal model with Parkinson's disease (PD). The dried root, also known as kushen in Chinese, has been used for hundreds of years in traditional Chinese medicines.
“Traditional Chinese medicines play an immeasurable role in the treatment of all kinds of diseases,” said thelead researcher Cheng-Peng Sun, a Dalian Medical University associate professor who is partnering with the Hammock lab on the PD research. For the past 35 years, Hammock, a distinguished professor who holds a joint appointment with the Department of Entomology and Nematology and the UC Davis Comprehensive Cancer Center, has researched enzyme inhibitors that dramatically reduce inflammation, inflammatory pain and neuropathic pain.
“We investigated the neuroprotective effects of S. flavescens in Parkinson's disease based on the neuroinflammation,” Sun explained. “Our extensive studies indicated that kurarinone possesses several pharmacological effects, including anti-inflammatory and antioxidative activities.”
The research, titled “Kurarinone Alleviated Parkinson's Disease via Stabilization of Epoxyeicosatrienoic Acids in Animal Model (Mice),” may lead to an effective therapy for PD, a progressive neurogenerative or brain disorder which affects more than 10 million people worldwide, including a million in the United States, according to the Mayo Clinic. Most PD patients are 65 or over and most are men. There is no cure.
“Basically, kurarinone targets the soluble epoxide hydrolase (sEH), which is a key regulatory enzyme involved in the metabolism of fatty acids, and inhibitors of the sEH enzyme resolve neuroinflammation,” said Professor Hammock, corresponding author. “The enzyme regulates a newly studied class of natural chemical mediators, which in turn regulates inflammation, blood pressure and pain.”
“We have known for a number of years that the soluble epoxide hydrolase inhibitors, now in human safety trials, are active in reducing the development of Parkinson's disease in several rodent models,” Hammock said. “The evidence for this is quite strong, particular based on work of our longterm collaborator Kenji Hashimoto at Chiba University in Japan. Certainly, Parkinson's disease is one of our targets for the sEH inhibitors, but the regulatory path is slow and expensive. This path becomes much faster for a natural product, so the discovery of this natural product from Cheng-Peng's laboratory potentially offers relief to patients far faster than a classical pharmaceutical.”
“In addition to its use as a natural product for treating Parkinson's disease, kurarinone provides a new model for the design of still more active compounds to block the neuroinflammation associated with multiple neurodegenerative diseases where sEH inhibitors have shown efficacy in rodent models including Alzheimer's, autism, and other disorders,” Hammock said. “The fact that kurarinone binds in the sEH enzyme in an adjacent but non-identical site opens the door to new synthetic drugs for these diseases.”

Co-author Christophe Morisseau, a biochemist in the Hammock lab, performed the enzyme kinetics, demonstrating the potency of the compound and how it interacts with the enzyme. “This research is important in two ways,” he said. “In lay terms, it demonstrates the use of a natural compound to treat Parkinson's disease. Right now, there is no effective treatment for this disease, so this is pretty cool. And we show that the compound used has a novel mechanism of inhibiting sEH compared to the previous inhibitors published.”
UC Davis Health System neurologist and School of Medicine Professor Lin Zhang, who is known for his PD expertise (he was not involved in the study), praised the research as novel and “Although we now have multiple medications to manage the debilitating symptoms of Parkinson's disease, we still don't have a way to stop the progression of the disease, not to mention having a cure,” said Zhang, who treats PD patients. “The conventional wisdom believes the reason for that is that we have been only treating the symptoms, not the cause of the disease. One of the contributing causes, as evidenced recently, has been neuroinflammation.”
A common Parkinson model comes from mice treated with MPTP (1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine). Tragically this deadly drug was discovered as an impurity in a recreational “This paper shows that when parkinsonian mice were treated with the natural product kurarinone, their Parkinson-like behaviors were significantly alleviated by attenuation of neurotoxicity,” Zhang said. “The same natural product was able to suppress sEH activities selectively so much so that neuroinflammation was markedly ameliorated. Furthermore, when the same models had their sEH gene knocked out, kurarinone did not provide additional protection against Parkinsonism.”
“This paper shows that kurarinone, a natural product, is able to alleviate Parkinson symptoms,” Zhang pointed out. “The mechanism for that has something to do with the fact that kurarinone targets soluble epoxide hydrolase (sEH) which mediates neuroinflammation. Products capable of inhibiting sEH like kurarinone can provide a novel, yet promising, mechanism to reduce neuroinflammation, subsequently treating neurodegenerative disorders including PD at its core.”
Added Zhang: “These findings presented in this paper help to solidify the candidacy of sEH as a key player of PD pathogenesis via neuroinflammation, underscoring the role of sEH inhibitors as a new class of anti-neuroinflammatory pharmaceuticals treating neurodegenerative disorders including PD.”
What's the next step?
“We hope that the natural herbal medicine will offer some relief from Parkinson's disease,” said Sun.
Added Morisseau: “We also hope to increase kurarinone levels in the plant and ensure that the extracts are nontoxic and effective. Possibly we can even find a food plant that is effective.”
Hammock lab researcher Sung Hee Hwang, an organic chemist, has been making small molecule inhibitors for Parkinson's disease, “and the crystal structure of sEH bound to kurarinone will be a great help to him,” Hammock said. “He has been working with Jogen Atone who is just finishing his doctorate in the UC Davis Pharmacology Toxicology program working on basic aspects of Parkinson's disease and environmental chemicals that may cause it.”
Sophora (the Arabic name for a pea-flowered tree) is a genus of about 45 species of evergreen trees and shrubs in the pea family, Fabaceae. The species are native to southern Asia, Australasia, various Pacific islands, western South America, the western United States, Florida and Puerto Rico. About fifteen of these species have a long history of use in traditional Chinese
“Now that we have a lead structure, we hope to screen related species for related compounds and efficacy,” Morisseau said.
“Parkinson's disease occurs when nerve cells in the basal ganglia, an area of the brain that controls movement, become impaired and/or die,” according to the National Institute on Aging (NIA). “Normally, these nerve cells, or neurons, produce an important brain chemical known as dopamine. When the neurons die or become impaired, they produce less dopamine, which causes the movement problems of Parkinson's. Scientists still do not know what causes cells that produce dopamine to die.”
“One clear risk factor for Parkinson's disease is age,” NIA says. “Although most people with Parkinson's first develop the disease at about age 60, about 5 to 10 percent of people with Parkinson's have ‘early-onset' disease, which begins before the age of 50. Early-onset forms of Parkinson's are often, but not always, inherited, and some forms have been linked to specific gene mutations.”
Hammock expressed hope that a variety of research pathways, such as the one resulting in kurarinone, “can lead to therapies, preventions and cures of Parkinson's disease and other neuroinflammatory problems associated with aging.”
Contact:
Bruce Hammock, bdhammock@ucdavis.edu


- Author: Kathy Keatley Garvey
Water balloons, water guns, super sprayers, and buckets prevailed when dozens of scientists participated in the 15th annual Bruce Hammock Lab Water Balloon Battle on the Briggs Hall lawn at the University of California, Davis.
The July event, also known as "Bruce's Big Balloon Battle at Briggs," proved to be an international soakfest. That's because the 28 researchers in the Hammock lab hail from seven countries: the United Stares, China, France, Ukraine, Lebanon, Japan and Korea. They include postdoctoral scholars, researchers, graduate students, visiting scholars, visiting graduate students, visiting summer students, short-term visiting scholars and student interns.
The annual battle amounts to 15 minutes, or "15 Minutes of Aim." That's how long it takes for the some 40 water warriors to toss 2,000 water balloons. Joining in were scientists from the Aldrin Gomes lab, UC Davis Department of Neurobiology, Physiology and Behavior; Frank Zalom lab of the UC Davis Department of Entomology and Nematology; and the UC Davis Department of Mathematics, plus family and friends.
Hammock, a UC Davis distinguished professor who holds a joint appointment with the UC Davis Department of Entomology and the UC Davis Comprehensive Cancer Center, hosts the annual event in mid-July when triple-digit temperatures strike the campus. It's an opportunity for the lab members--who work hard throughout the year and play hard for 15 minutes--to engage in a little fun and camaraderie. The thirsty lawn benefits, too.
First the water warriors fill the balloons in an assemblyline procedure, and at exactly 3 p.m., the soakfest begins. As the H2O dwindles, they empty buckets at unsuspecting targets. The last part: picking up every single balloon remnant from the lawn.
Hammock, trained as a entomologist, chemist and toxicologist--and who now focuses his research on human health, is recognized for his work on using natural chemical mediators to control inflammation and intractable pain. He co-discovered the soluble epoxide hydrolase, and many of his more than 1100 publications and patents are on the P450 branch of the arachidonate cascade where the soluble epoxide hydrolase (sEH) degrades natural analgesic and anti-inflammatory compounds.
Hammock, an alumnus of UC Berkeley with a doctorate in entomology, joined the UC Davis faculty in 1980. He is the founding director (1987-present) of the UC Davis NIEHS (National Institute of Environmental Health Sciences) Superfund Research Program and is a founding member (1990-present) of the UC Davis Comprehensive Cancer Center. He has directed the UC Davis NIH/NIEHS Combined Analytical Laboratory for 25 years.
Highly honored by his peers, Hammock is a fellow of the National Academy of Inventors, which honors academic invention and encourages translations of inventions to benefit society. He is a member of the U.S. National Academy of Sciences, a fellow of the Entomological Society of America, and the recipient of the Bernard B. Brodie Award in Drug Metabolism, sponsored by the America Society for Pharmacology and Experimental Therapeutics. He is the first McGiff Memorial Awardee in Lipid Biochemistry. The Eicosanoid Research Foundation recently honored him for work on oxidized lipids.
But on one day in July--for 15 minutes--noted academician Bruce Hammock leaves his Briggs Hall office and transforms into an elite water warrior. He's practiced for 15 years, 15 minutes at a time.
"Bruce has a good aim," said Christophe Morisseau, a Hammock lab researcher who coordinates the annual battles.



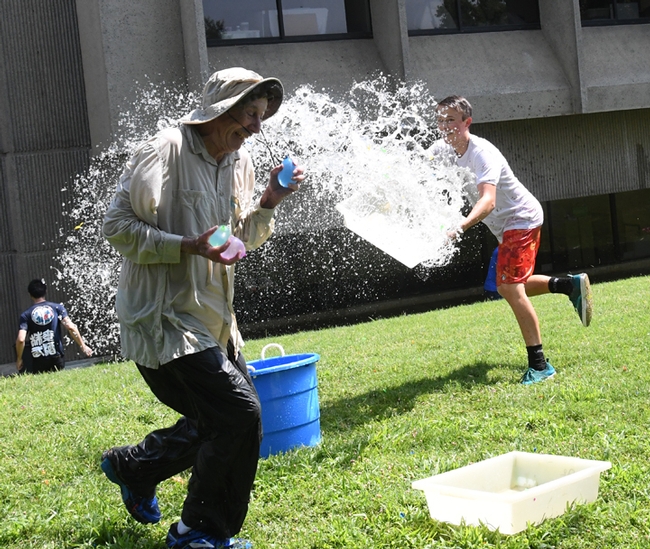




- Author: Kathy Keatley Garvey

Earlier research by the Judah Folkman laboratory of Harvard Medical School showed that cutting off blood vessels that feed a cancerous tumor can stop its growth.
The seven-member research team—five from the Bruce Hammock laboratory of UC Davis—“characterized a novel lipid signaling molecule that can change fundamental biological processes involved in our health and disease,” said lead author and researcher Amy Rand. “We've found that a novel product derived from the metabolism of omega-6 fatty acids stimulates angiogenesis, which may contribute to enhanced tumor growth by providing tumors with oxygen and nutrients.”
“As a highly regulated process, angiogenesis is critical for wound healing and development, but many diseases result in unregulated angiogenesis, including cancer,” explained Rand, a postdoctoral fellow in the lab of Bruce Hammock, a distinguished professor who holds a joint appointment with UC Davis Department of Entomology and Nematology and the UC Davis Comprehensive Cancer Center. “We may be able to control angiogenesis to stimulate wound healing when necessary, but also block tumor growth in patients. Diseases that rely on angiogenesis may be able to be treated in part by changes in dietary lipid exposure or by controlling levels of these metabolites through enzyme inhibitors that block their formation.”
The research, published April 10 in the Proceedings of the Natural Academy of Sciences (PNAS), explains, in part, why inhibiting the soluble epoxide hydrolase (sEH) in some systems is angiogenic whereas combining sEH inhibition with the inhibition of cyclooxygenase (COX) enzymes is dramatically antiangiogenic, which in turn may suppress tumor growth.
“There's uncertainty regarding the link between unsaturated fats and cancer, due to ongoing conflicts between scientific studies and insufficient data,” Rand said. “Because of this, there is a major gap in our understanding of how these essential dietary fats affect our health. We used tools to detect and characterize unknown metabolites from omega-6 unsaturated fats and determined their effect on angiogenesis, to address at least a small part of this uncertainty by focusing on how these fats contribute to cancer tumor growth.”
Hammock, who holds a joint appointment in the UC Davis Department of Entomology and Nematology and the UC Davis Comprehensive Cancer Center, said the research, titled “Cyclooxygenase-Derived Proangiogenic Metabolites of Epoxyeicosatrienoic Acids
Holds long term hope for cancer patients and those afflicted with heart, eye and other diseases. The team also included Christophe Morisseau, Bogdan Barnych, and Kin Sing Stephen Lee all of the UC Davis Department of Entomology and Nematology and UC Davis Comprehensive Cancer Center; Tomas Cajka of the UC Davis Genome Center; and Dipak Panigraphy of Harvard Medical School. Lee is now an assistant professor at Michigan State University.
“Pro and anti-angiogenic therapy can potentially help millions of people worldwide in various diseases such as heart, ulcers, eye and cancer as first demonstrated by Dr. Judah Folkman and his colleagues,” said Panigraphy, formerly of the Hammock lab and now with the Center for Vascular Biology Research, Beth Israel Deaconess Medical Center, Harvard Medical School, and the school's Department of Pathology.
“While the COX and sEH pathways can be targeted with drugs, their interaction is poorly understood,” Panigraphy said. “These studies by Rand et al demonstrate for the first time new specific mechanisms whereby targeting the sEH pathway can be both pro- and anti-angiogenic and has the potential to help patients with devastating diseases such as in the eye and cancer where blocking angiogenesis is desired.”
Rand, who received her doctorate in chemistry from the University of Toronto, Canada, in 2013, the same year she joined Hammock's biological analytical chemistry lab, said she's “always been interested in research that combines chemistry and biology to enhance our understanding of human health.”
Future work? “We aim to understand the direct involvement of these omega-6 fatty acid metabolites with cancer tumor growth and metastasis.”
Rand last year received the $100,000 Judah Folkman Fellowship for Angiogenesis Research from the American Association for Cancer Research. She won the highly competitive international award for her proposal, “Regulation of Cancer Angiogenesis from the Metabolism of Epoxy Omega-6 Fats.” Rand joined Hammock's biological analytical chemistry lab in 2013 and was a fellow on the Oncogenic Signals and Chromosome Biology T32 Training Grant, UC Davis Department of Microbiology and Molecular Genetics.
The late Judah Folkman (1933-2008), a Harvard Medical School professor considered the father of angiogenesis research, “is best known for pioneering the concept of blocking angiogenesis (the development of blood vessels) to control cancer growth," Hammock said. "This concept has resulted in a number of anti-cancer drugs and has had a major impact on cancer treatment. Of course, blood vessel development is also critical for survival."
Folkman discovered that cutting off the blood vessels that feed the tumor can stop cancer tumor growth. His revolutionary work has led to the discovery of a number of therapies based on inhibiting or stimulating neovascularization. Inhibitors of the sEH pathway are moving toward human trials to control neuropathic pain, but if combined with nonsteroidal anti-inflammatory drugs can block tumor growth by blocking angiogenesis. So Dr. Sung Hee Hwang combined inhibitors of both pathways into one molecule which is being investigated in cancer models at the UC Davis Cancer Center by Dr. Paul Henderson and Northwestern University Medical School by Dr. Guang-yu Yang.
Hammock directs the campuswide Superfund Research Program, National Institutes of Health Biotechnology Training Program, and the National Institute of Environmental Health Sciences (NIEHS) Combined Analytical Laboratory.
This work was supported by NIEHS and the NIEHS Superfund Program; and two of Rand's grants: the Oncogenic Signals and Chromosome Biology T32 Training Grant, NIH/NIEHS; and her 2016 AACR Judah Folkman Fellowship for Angiogenesis Research.

- Author: Kathy Keatley Garvey

Researchers at the Huazhong University of Science and Technology, Wuhan China, used the drug developed at UC Davis to show that the neurofibrillary pathology of an Alzheimer's disease-related protein could be dramatically reduced. Their work was published in December in the Journal of Huazhong University of Science and Technology.
“They further demonstrated the mechanism of action of the UC Davis drug in blocking the oxidative stress-driven phosphorylation events associated with Alzheimer's disease,” Hammock said. The UC Davis drug stabilizes natural anti-inflammatory mediators by inhibiting an enzyme called soluble epoxide hydrolase (sEH) discovered at UC Davis and recently spotlighted in the Proceedings of the National Academy of Sciences and the National Institutes of Health's PubMed.
“I was thrilled to see this paper on tau phosphorylation from Huazhong University shows that our drug could block a key event and a key enzyme called GSK-3 beta thought critical in the development of Alzheimer's disease,” said Hammock, who holds a joint appointment in the UC Davis Department of Entomology and Nematology and the UC Davis Comprehensive Cancer Center.
“We were planning to do this study, but having another laboratory do it with our compound was even better,” he said. “Since our publication last year in PNAS that showed UC Davis soluble epoxide hydrolase inhibitors both prevented and reversed depression, we have been excited about trying to block the development of Alzheimer's disease.”
The PNAS paper, “Gene Deficiency and Pharmacological Inhibition of Soluble Epoxide Hydrolase Confers Resilience to Repeated Social Defeat Stress,” was co-authored by a 13-member research team led by Hammock and Kenji Hashimoto of Chiba University Center's Division of Clinical Neuroscience, Japan. They found that sEH plays a key role in the pathophysiology of depression, and that epoxy fatty acids, their mimics, as well as sEH inhibitors could be potential therapeutic or prophylactic drugs for depression and several other disorders of the central nervous system. Co-authors of the paper included Hammock lab researchers Christophe Morisseau, Jun Yang and Karen Wagner.
Hammock credited several UC Davis colleagues for their work leading to the publications. Research from the labs of Liang Zhang and Qing Li at the University of Hawaii--Qing is a former UC Davis doctoral student--pointed out some of the mechanisms involved in cognitive decline which associate professor Aldrin Gomes of the UC Davis Department of Neurobiology, Physiology and Behavior and Fawaz Haj of the UC Davis Department of Nutrition “have shown to be blocked by the natural metabolites stabilized by the UC Davis drugs,” Hammock said.
One of the Hammock lab drugs is moving toward human clinical trials for neuropathic pain through a Davis-based company, EicOsis, LLC, and the financial support of the Blueprint Program through NIH's National Institute of Neurological Disorders and Stroke. Hammock founded the company to develop inhibitors to the soluble epoxide hydrolase, a key regulatory enzyme involved in the metabolism of fatty acids, to treat unmet medical needs in human and animals.
“The clinical back-up candidate at EicOsis penetrates the blood brain barrier and should be a perfect compound to test if this class of chemistry can prevent cognitive decline and Alzheimer's disease,” Hammock said.
The National Institute of Environmental Health Sciences, National Institutes of Health, funded the research.
Highly honored by his peers, Hammock is a fellow of the National Academy of Inventors, which honors academic invention and encourages translations of inventions to benefit society. He is a member of the U.S. National Academy of Sciences, a fellow of the Entomological Society of America, and the recipient of the Bernard B. Brodie Award in Drug Metabolism, sponsored by the America Society for Pharmacology and Experimental Therapeutics. He directs the campuswide Superfund Research Program, National Institutes of Health Biotechnology Training Program, and the National Institute of Environmental Health Sciences (NIEHS) Combined Analytical Laboratory.

- Author: Kathy Keatley Garvey

“We think that this research will lead to a very positive outcome to improve the lives of cystic fibrosis patients,” said co-author Bruce Hammock, distinguished professor in the UC Davis Department of Entomology and Nematology who holds a joint appointment with the UC Davis Comprehensive Cancer Center.
The research, published in the current edition of the Proceedings of the National Academy of Sciences, links a newly discovered class of bacterial enzymes to battling cystic fibrosis, a progressive, genetic disease characterized by persistent lung infections and inability to breathe normally.
Senior author Jennifer Bomberger of the Department of Microbiology and Molecular Genetics, University of Pittsburgh School of Medicine explained that the opportunistic bacterium, Pseudomonas aeruginosa, outcompetes other microorganisms in a cystic fibrosis patient's lungs and establishes a stronghold.

The scientific discovery could lead to new therapies that would interrupt or correct the bacterial sabotage, Hammock and Bomberger said.
“This paper is the outcome of an exciting and interdisciplinary project,” said Hammock, who directs the UC Davis Superfund Program financed by the National Institutes of Health's National Institute of Environmental Health Sciences (NIH-NIEHS).
“It started several years ago with the NIEHS Superfund Program funding both a group at Dartmouth and at UC Davis. A very productive and exciting collaboration resulted in looking at how to mitigate the effects of environmental chemicals on human health. Our collaborative work led to this joint publication which yields exciting hope for cystic fibrosis patients.”
Bomberger continues to work on the biology of the system while the Dartmouth and Davis groups have developed inhibitors of the action of CIF to stabilize pro-resolving mediators, reduce inflammation, and control periodic flare ups of bacterial infections.
"It will be key to devise a way to remove P. aeruginosa's ability to capitalize on the body's natural inflammatory response, without eliminating that response," said Bomberger. "Inflammation is happening for a reason—to clear infection. We just need it to temper the response when it is not effectively doing its job or is no longer needed."
Other co-authors of the paper include Hammock lab members Christophe Morisseau and Jun Yang, both from the UC Davis Department of Entomology and Nematology and UC Davis Comprehensive Cancer Center. .Institutions involved in the study also included the Harvard School of Medicine.




