- Author: Kathy Keatley Garvey

The soldiers called the mosquitoes "gallinippers."
Physicians had not yet linked malaria to Anopheles mosquitoes. They believed "humidity" or “swamp effluvia" caused what they called "intermittent fever."
Soldiers who contracted "intermittent fever" complained of "ague" (fever and chills) or "the shakes."
Sam, a towering farm boy from Linn., Mo., was 18 when he enlisted in the Union Army. Company commanders selected him as the color bearer for three reasons: his height (6' 3"), his strength (hoisting the flag and flying it high) and his courage (front lines)
"Being a color bearer (aka carrying the flag), was a prestigious and important role in the Army. Not only were you carrying the symbol of what you were fighting for, the flag was any easy mark for soldiers to organize around," according to an article written in a National Museum of Civil War Medicine post by Amelia Grabowski, the outreach and education coordinator at the National Museum of Civil War Medicine and the Clara Barton Missing Soldiers Office Museum.
"When one color-bearer fell, another immediately took his place. For instance, Colonel D. K. Mcrae of the 5th North Carolina Infantry, Commanding Brigade recorded this about the Battle of Williamsburg: My color bearer was first struck down, when his comrade seized the flag, who fell immediately. A third took it and shared the same fate; then Capt. Benjamin Robinson, of Company A, carried it until the staff had shivered to pieces in his hands."
"...The flags made them (color bearers) easy and enticing targets," Grabowski wrote.
Young Samuel carried the flag in three of the bloodiest battles of the Civil War: the Battle of Lookout Mountain, and the battles of Chicamauga and Chattanooga. A musket tore a hole in his flag but he emerged from the Civil War physically unscathed.
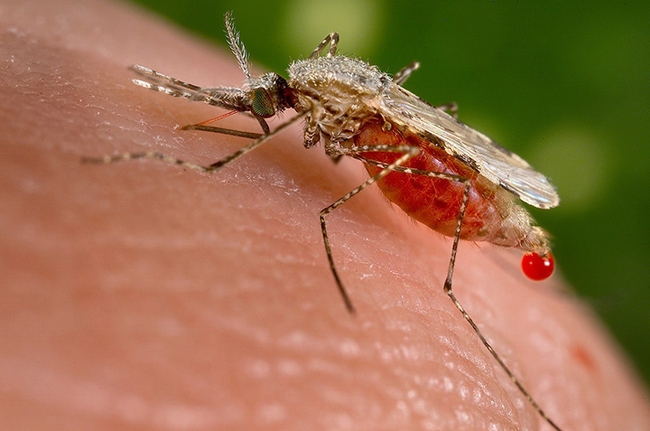
"The diagnosis of malaria at the time of the Civil War was made by symptoms and not the laboratory tests we use today," wrote Lloyd Klein and Eric Wittenberg of San Francisco, in Hektoen International, a Journal of Medical Humanities. "Nineteenth-century physicians diagnosed malaria as a recurrent, intermittent, or 'periodic' fever and categorized it according to how often fever spikes or 'paroxysms' occurred. A 'quotidian' fever occurs once every twenty-four hours, a 'tertian' every forty-eight, and a 'quartan' every seventy-two."
The authors related that malaria killed some 30,000 Civil War soldiers. Among Union soldiers, some 10,000 died of malaria, and records show more than a million cases of the disease.
Ironically, after surviving the Civil War, Samuel Davidson Laughlin died from blood poisoning when a splinter lodged in his hand when he was carrying an armload of firewood into the family home in Castle Rock, Wash. The color bearer, the husband, the father, and the grandfather died Feb. 24, 1910 in an Oregon hospital. He is buried on a knoll overlooking the historic round barn (now in the National Register of Historic Places) that he built in 1883.
His gravestone reads simply: "Gone, but not forgotten."

- Author: Kathy Keatley Garvey

Enter Filipa Rijo-Ferreira, a UC Berkeley School of Public Health (BPH) assistant professor who specializes in parasitology and circadian rhythms.
She'll present a UC Davis Department of Entomology and Nematology seminar at 4:10 p.m., Wednesday, Oct. 19 on "Circadian Rhythms in Parasitic Diseases" in 122 Briggs Hall. Her seminar also will be virtual. The Zoom link is https://ucdavis.zoom.us/j/95882849672. Host is molecular geneticist and physiologist Joanna Chiu, professor and vice chair of the UC Davis Department of Entomology and Nematology.
"Malaria's main symptom is the periodic fevers experienced by patients, fevers that ‘come and go' at certain times of the day and are a consequence of synchronized parasite rhythms," Rijo-Ferreira says in her abstract. "In humans, circadian clocks regulate multiple aspects of physiology, including sleep-wake cycles, metabolism, and immune defense. Circadian biology leads to body rhythms experienced by the pathogens that infect humans. In addition to sensing host rhythms, we recently discovered that parasites which cause devastating health burdens such as malaria and sleeping sickness diseases also have their own intrinsic clocks. The clocks of parasites regulate core biological functions from metabolism to the cell cycle, and the discovery of the existence of their clocks serves as an opportunity to access the molecular mechanisms regulating their rhythmic biology."
A native of Lisbon, Portugal, Rijo-Ferreira joined the UC Berkeley Public Health faculty in January 2022. She describes herself as a "scientist passionate about the complex daily host-parasite interactions and how parasites evolved circadian clocks to anticipate environmental cycles." She recently authored "The Malaria Parasite Has an Intrinsic Clock," published in Science magazine.

"Our lab is interested in parasitic infections and we study them under the lenses of time of day," Rijo-Ferreira wrote on her lab website. "Our rhythmic world has been a driving force for organisms to evolve a molecular clock to anticipate such daily rhythms. Similarly, our own circadian biology leads to physiological rhythms that parasites experience.We study the single-celled parasites Plasmodium spp. that causes malaria, and Trypanosoma brucei that causes sleeping sickness. We employ technical approaches spanning from next-generation sequencing, to cellular and behavioral assays to investigate the interactions of these parasites with their hosts.Our work seeks to understand how circadian rhythms modulate host-parasite-vector interactions and identify opportunities in their rhythmic biology to treat parasitic infections
In an interview with BPH staff writer Eliza Partika, published in February 2022, she commented: "I am fascinated about our day and night cycles and how organisms evolved to anticipate them. I find it incredible that parasites, such as the ones that cause malaria, show a coordinated rhythmic pattern themselves, which underlies periodic fevers in infected individuals. Our research is aimed at understanding how this phenomenon is regulated molecularly, and how we can disrupt these rhythmic patterns to offset the infection."
"At BPH, we aim to set up a framework where we can explore the relationships between parasites, hosts, and the mosquitoes that serve as the vector of disease transmission, based on the time of day," Rijo-Ferreira related. "We hypothesize that the circadian rhythms of these three organisms need to be aligned in order for the parasite to cause an efficient infection. In fact, when rhythms are misaligned, there is a reduction in parasite levels. Thus, identifying the molecular players from host, parasite, and mosquito is essential to understanding this phenomenon and creating alternative strategies to manage deadly infections like malaria and sleeping sickness."
Rijo-Ferreira said she seeks to "bring to the attention the circadian aspect of infectious diseases and bring awareness of the potential benefits of time of day vaccination and drug treatment."
Emily Meineke, assistant professor of urban landscape entomology, UC Davis Department of Entomology and Nematology, coordinates the department's seminars for the 2022-23 academic year. All 11 seminars will take place both person and virtually at 4:10 p.m. on Wednesdays in Room 122 of Briggs Hall except for the Nov. 9th and Dec. 7th seminars, which will be virtual only, she said. (See list of seminars)
For further information on the seminars or to resolve any technical difficulties with Zoom, contact Meineke at ekmeineke@ucdavis.edu.

- Author: Kathy Keatley Garvey

Wait, there's more! "Not So Heartless: Functional Integration of the Immune and Circulatory Systems of Mosquitoes."
This may not be the proverbial heart-stopping seminar, but it promises to be an eye opener by a medical entomologist and captivating speaker.
Julián Hillyer, associate professor of biological sciences, Vanderbilt Institute for Infection, Immunology and Inflammation, Nashville, Tenn., will deliver that seminar at 4:10 p.m., Wednesday, Oct. 23, in 122 Briggs Hall, as part of the weekly UC Davis Department of Entomology and Nematology seminars.
"Mosquitoes--like all other animals--live under constant threat of infection," Hillyer says in his abstract. "Viral, bacterial, fungal, protozoan and metazoan pathogens infect mosquitoes through breaches in their exoskeleton and following ingestion. Because these pathogens pose a threat to their survival, mosquitoes have evolved a powerful immune system."
In his seminar, Hillyer will present his laboratory's work characterizing the circulatory and immune systems of the African malaria mosquito, Anopheles gambiae. "Specifically," he says. "the talk will describe the structural mechanism of hemolymph (insect blood), circulation in different mosquito life stages, and the role that immune cells, called hemocytes play in the killing of pathogens by phagocytosis, melanization and lysis. Then I will describe the functional integration of the circulatory and immune systems a process that is manifested differently in larvae and adults. Specifically, the infection of an adult mosquito induces the aggregation of hemocytes at the abdominal ostia (valves) of the heart--where they sequester and kill pathogens in areas of high hemolymph flow--whereas the hemocytes of larvae aggregate instead on respiratory structures that flank the posterior in current openings of the heart."
"This research," Hillyer explains, "informs on the physiological interaction between two major organ systems and uncovers parallels between how the organ systems of invertebrate and vertebrate animals interact during the course of an infection."
What does the mosquito heart look like? Check out former Vanderbilt graduate student Jonas King's prize-winning image--a fluorescent image of the heart of a mosquito. It won first place in Nikon's "Small World'" photomicrography competition in 2010. King's image shows a section of the tube-like mosquito heart magnified 100 times. At the time he was a member of Hillyer's research group and is now an assistant professor at Mississippi State University.
In a piece by David Salisbury of Vanderbilt News, Hillyer related that "Surprisingly little is known about the mosquito's circulatory system despite the key role that it plays in spreading the malaria parasite. Because of the importance of this system, we expect better understanding of its biology will contribute to the development of novel pest- and disease-control strategies.”
"The mosquito's heart and circulatory system is dramatically different from that of mammals and humans," wrote Salisbury in the Oct. 15, 2010 piece. "A long tube extends from the insect's head to tail and is hung just under the cuticle shell that forms the mosquito's back. The heart makes up the rear two-thirds of the tube and consists of a series of valves within the tube and helical coils of muscle that surround the tube. These muscles cause the tube to expand and contract, producing a worm-like peristaltic pumping action. Most of the time, the heart pumps the mosquito's blood—a clear liquid called hemolymph—toward the mosquito's head, but occasionally it reverses direction. The mosquito doesn't have arteries and veins like mammals. Instead, the blood flows from the heart into the abdominal cavity and eventually cycles back through the heart."
“The mosquito's heart works something like the pump in a garden fountain,” Hillyer told Salisbury.
Hillyer was a Vanderbilt Chancellor Faculty Fellow (2016-2018) and was awarded the 2015 Henry Baldwin Ward Medal by the America Society of Parasitologists. He was elected to the Council of the American Society of Parasitologists, serving from 2012-2016. Other recent awards: the 2011 Jeffrey Nordhous Award for Excellence in Undergraduate Teaching and the 2012 Recognition Award in Insect Physiology, Biochemistry and Toxicology from the Southeastern Branch of the Entomological Society of America.
Hillyer received his master's degree and doctorate from the University of Wisconsin-Madison under the mentorship of Ralph Albrecht and Bruce Christensen, respectively. He completed a postdoctoral fellowship under the mentorship of Kenneth Vernick at the University of Minnesota, now with Institut Pasteur. In 2007, Hillyer moved to Nashville, Tenn. to establish Vanderbilt University's mosquito immunology and physiology laboratory. (See more.)
The Hillyer Lab is interested in basic aspects of mosquito immunology and physiology, focusing on the mechanical and molecular bases of hemolymph (blood) propulsion, and the immunological interaction between mosquitoes and pathogens in the hemocoel (body cavity)," according to his website. "Given that chemical and biological insecticides function in the mosquito hemocoel, and that disease-causing pathogens traverse this compartment prior to being transmitted, we expect that our research will contribute to the development of novel pest and disease control strategies."
Host is Olivia Winokur, doctoral student in the Chris Barker lab. Community ecologist Rachel Vannette, assistant professor, Department of Entomology and Nematology, coordinates the weekly seminars. (See list of seminars)

- Author: Kathy Keatley Garvey

When the United Nations meets Sept. 21 in New York, they want the UN to reframe its action on the global antimicrobial drug resistance (AMR) crisis.
It's crucial. How crucial is it?
Antimicrobial drug resistance threatens both personal and planetary health and the issue is as crucial as the global threat of climate change, Carroll says.
In a paper titled “Use Antimicrobials Wisely,” published in the current edition of Nature, a nine-member international research team, including Carroll, explained their advocacy.
“We're concerned about what will happen if the proposed UN solutions focus mainly on incentives for new drug development, at a time when the drug industry itself is abandoning those efforts against infectious disease due to AMR,” said Carroll, who co-leads the international group on resistance to pesticides and antimicrobial drugs. He founded and directs the Institute for Contemporary Evolution, Davis, and is affiliated with the Sharon Lawler lab, UC Davis Department of Entomology and Nematology.
The paper, published in the Comment section, is the first product from a two-year working group sponsored by the National Socio-Environmental Synthesis Center in Annapolis, Md. “We are taking a similar socio-environmental approach in our concurrent work on pesticide stewardship,” Carroll said.
“While new drugs have a role, we think it's more important for society to learn how to steward pathogen susceptibility, so we develop that theme in the paper,” Carroll said. “And because we also depend on microbes for digestion, immunity, and general health, and microbes support ecosystem functioning through nutrient cycles and the maintenance of soil and water quality, we further argue that our AM drug habits and waste streams threaten both personal and planetary health. “
Lead authors of the paper are Peter Jorgensen of Stockholm, Sweden, and Didier Wernli of Geneva Switzerland. Jørgensen, who spent part of his Danish graduate program working with Carroll in Davis, is now a postdoctoral researcher at the Royal Swedish Academy of Science, Stockholm.
Carroll described AMR as more than a medical dilemma—it's a socio-ecological problem. “The vulnerability of pathogens to antimicrobial drugs is a communal resource, readily threatened by overuse, to be lost as a classic 'tragedy of the commons.' There is a lot of contemporary theory for social resilience in the face of socio-ecological challenges, and– linking to entomology– the early success of the pioneering management of Bt crop pest resistance evolution is an encouraging precedent.”
In its planetary health approach, the group seeks to be “more cognizant not only of preserving drug susceptibility in pathogenic microbes, but also protecting from wholesale destruction the community of microbes on which we depend for life,” Carroll said.
In the paper, the scientists pointed out that “Resistance affects animal and environmental health as well as human health, and so requires coordinated action across economic sectors. No single concern exemplifies this better than the high rate of antibiotic use in agriculture (largely as growth promoters or disease prevention).” They wrote that in the United States, 70 to 80 percent of all anti-microbials consumed are given to livestock.
An example of antimicrobial resistance involves the malaria mosquito, Anopheles gambiae. The World Health Organization (WHO) in a document, "Global Action Plan on Anti-Microbial Resistance," wrote:
"Antimicrobial resistance can affect all patients and families. Some of the commonest childhood diseases in developing countries – malaria, pneumonia, other respiratory infections, and dysentery – can no longer be cured with many older antibiotics or medicines. In lower- income countries, effective and accessible antibiotics are crucial for saving the lives of children who have those diseases, as well as other conditions such as bacterial blood infections. In all countries, some routine surgical operations and cancer chemotherapy will become less safe without effective antibiotics to protect against infections."
Expect to hear more about this alarming crisis--the global antimicrobial drug resistance crisis. Meanwhile, read the WHO Global Action Plan.

- Author: Kathy Keatley Garvey
You don't usually see "honey bees" and "malaria" in the same sentence.
That won't be the case, though, when Joseph DeRisi, a Howard Hughes Medical Institute investigator and professor and vice chair of the Department of Biochemistry and Biophysics, University of California, San Francisco, comes to the UC Davis campus to lecture on Monday, Jan. 9.
His presentation, "A Seminar in Two Acts: Honey Bees and Malaria," is from 10 to 11 a.m. in the main auditorium (Room 2005) of the Genome and Biomedical Sciences Facility.
The seminar, open to all interested persons, is sponsored by the Biological Networks Focus Group of the Genome Center. Host is Oliver Fiehn, professor in the Department of Molecular and Cellular Biology and the Genome Center.
DeRisi, a molecular biologist and biochemist, was named the recipient of a MacArthur Foundation Grant (also known as "the genius award") in 2004. In 2008, DeRisi won the Heinz Award for Technology, the Economy and Employment. Among his many accomplishments: he designed and programmed a groundbreaking tool for finding (and fighting) viruses -- the ViroChip, a DNA microarray that test for the presence of all known viruses in one step.
The DeRisi lab drew international attention last year with publications in Public Library of Science journals.
Malaria:
Chemical Rescue of Malaria Parasites Lacking an Apicoplast Defines Organelle Function in Blood-Stage Plasmodium falciparum (published in PLoS Biology, August 2011)
Honey Bees:
Temporal Analysis of the Honey Bee Microbiome Reveals Four Novel Viruses and Seasonal Prevalence of Known Viruses, Nosema, and Crithidia (published in PLoS One, June, 2011)
Among those working on the honey bee research and co-authoring the PLoS One paper was insect virus researcher Michelle Flenniken, a postdoctoral fellow in the Raul Andino lab at UC San Francisco and the recipient of the Häagen-Dazs Postdoctoral Fellowship in Honey Bee Biology at UC Davis.
Among DeRisi's collaborators on malaria research is UC Davis molecular biologist Shirley Luckhart, professor in the Department of Medical Microbiology and Immunology and an advisor in the Entomology Graduate Program.
DeRisi, who received his Ph.D. in biochemistry in 1999 from Stanford University, does amazing work.
He's a genius, to be sure.
Check out these links:
Joseph DeRisi Lab, UC San Francisco
Joe DeRisi: Biochemist (featured in TED ("Technology, Entertainment, Design" is a nonprofit devoted to Ideas Worth Spreading.)
Conversation with Joe DeRisi (New York Times)
Solving Medical Mysteries (YouTube)
Hunting the Next Killer Virus (YouTube)
Joseph DeRisi: Howard Hughes Medical Institute
Joseph DeRisi in Wikipedia




