- Author: Kathy Keatley Garvey
Embargo lifts at 10 a.m., Pacific Time


An inhibitor to the enzyme, soluble epoxide hydrolase (sEH), discovered in the Hammock lab, prevented the eye disease in diabetic mice, Fleming said.
The paper, “Inhibition of Soluble Epoxide Hydrolase Prevents Diabetic Retinopathy,” involving six years of research and 22 scientists, is published today (Dec. 6) in the journal Nature.
"This has been a long but exciting project where Dr. Fleming's team used tools developed to study the biology of fatty acid epoxides to probe the fundamental mechanism of diabetic retinopathy,” said co-author Hammock, a distinguished professor of entomology who holds a joint appointment with the UC Davis Department of Entomology and Nematology and the UC Davis Comprehensive Cancer Center “This work has targeted many possible sites for intervention that could preserve vision, and one such target is using inhibitors of the soluble epoxide hydrolase which block diabetic retinopathy in mice.”
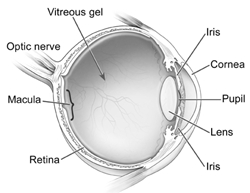
The eye generates a dihydroxy metabolite from polyunsaturated fatty acids that initiates pericyte loss and breakdown of the endothelial barrier function in the eye, the scientists said. This leads to vascular edema and ultimately to a proliferation of new blood vessels and loss of vision.
The small molecule which initiates this process is a diol of a long chain poly unsaturated fatty acid produced by sEH, the researchers said. The enzyme converts an anti-inflammatory epoxy fatty acid into the pro inflammatory and in this case, toxic diol. The research team demonstrated this process and the cellular mechanism involved in diabetic mice and in transgenic mice that over-produce the sEH enzyme.
They were able to block the process by inhibiting the sEH enzyme. The expression of the sEH enzyme also increased with severity of diabetic retinopathy in human patients.
“The expression of the soluble epoxide hydrolase gene was shown to increase in the retinas of human patients with the severity of the disease with non-proliferative diabetic retinopathy,” Hammock said. “Thus, there appears a connection to human medicine.”
Diabetic retinopathy is the most common diabetic eye disease and a leading cause of adult blindness. Chronically high blood sugar from diabetes damages the tiny blood vessels in the retina, leading to diabetic retinopathy, according to the National Eye Institute (NEI) of the National Institutes of Health. The blood vessels can leak fluid or hemorrhage, distorting vision. NEI officials predict that the number of Americans with diabetic retinopathy will nearly double from 7.7 million in 2010 to 14.5 million by 2050.
Fleming said the sEH enzyme generates a toxic metabolite, but when the enzyme is inhibited, eye disease is prevented.
Earlier work reported in the Proceedings of the National Academy of Sciences from the Kip Connor laboratory at Harvard University showed that inhibiting the soluble epoxide hydrolase preserves fatty acid epoxides which reduce the late or proliferative stages of diabetic retinopathy and macular degeneration. Now the Fleming team used the same soluble epoxide hydrolase inhibitors to block production of a pro inflammatory mediator that initiates the early stages of vascular permeability and inflammation of the retina.
Connor, an assistant professor of ophthalmology at Harvard Medical School, praised the work as bringing to light ”a previously unknown mechanism of action.” Said Connor: “The identification by the laboratories of Drs. Fleming and Dr. Hammock that 19,20-dihydroxydocosapentaenoic acid, a product of soluble epoxide hydrolase (sEH) activity, as a key regulator of pericyte loss and endothelial barrier breakdown has brought to light a previously unknown mechanism of action in the induction of diabetic retinopathy. Moreover, the authors clearly show that inhibition of sEH blocks formation of this degenerative lipid metabolite thereby halting disease progression, which is of vital interest for the potential management of this blinding disease.
Mehran Moghaddam and David Grant, then with the Hammock lab, demonstrated that the diol of the fatty acid linoleate produced by the soluble epoxide hydrolase was highly toxic to cells leading to vascular permeability and sepsis. They published their work in 1997 in Nature Medicine.
"It is interesting how discoveries of years ago resurface as a critical lead in another disease indication,” commented Moghaddam. “It certainly seems hopeful we will be able to treat blindness resulting from severe diabetes."
The Hammock laboratory has published almost 900 peer-reviewed papers on the sEH enzyme, discovered while Hammock and Sarjeet Gill (now of UC Riverside) were researching insect developmental biology and green insecticides at UC Berkeley. The work, begun in 1969, led to the discovery that many regulatory molecules are controlled as much by degradation as by biosynthesis, Hammock said. These epoxy fatty acid chemical mediators control blood pressure, fibrosis, immunity, tissue growth, pain and inflammation to name a few processes, and now Fleming's team has shown the diols products from these epoxides can cause diabetic retinopathy.
For many years Gill and Hammock were alone in studying this enzyme but today its importance is well recognized in mammalian biology, with more than 17,000 peer-reviewed papers in the area. Hammock credits the National Institute of Environmental Health Sciences (NIEHS) for supporting research in this area since the 1970s.
A Davis-based company, EicOsis, has received a large grant from the U.S. National Institutes of Health to move inhibitors to the clinic to treat diabetic neuropathic pain. “We are developing a non opiate analgesic to treat the chronic pain often associated with diabetes,” said William Schmidt, vice president of clinical development at EicOsis. "It would be wonderful if the came drug also could be used to prevent the blindness driven by diabetes.
Contacts:
Bruce Hammock at bdhammock@ucdavis.edu
Ingrid Fleming at Fleming@vrc.uni-frankfurt.de
- Author: Kathy Keatley Garvey

Hammock, a distinguished professor who holds a joint appointment with the UC Davis Department of Entomology and Nematology and the UC Davis Comprehensive Cancer Center, just received a copy of the magazine listing the research as No. 76. The space exploration of Pluto made No. 1. The top stories encompassed space exploration, medicine, technology, paleontology and the environment.
The UC Davis research was singled out for “Endoplasmic Reticulum Stress in the Peripheral Nervous System is a Significant Driver of Neuropathic Pain,” published in July 2015 in the Proceedings of the National Academy of Sciences. (See UC Davis news story)
Lead researchers Bora Inceoglu of the Hammock lab UC Davis Department of Entomology and Nematology/UC Davis Comprehensive Cancer Center, and Ahmed Bettaieb, then of the Fawaz Haj lab, Department of Nutrition, pinpointed the key mechanism that causes neuropathic pain--a complex, chronic and difficult-to-treat pain caused by nerve injuries from trauma or from such diseases as diabetes, shingles, multiple sclerosis and stroke.
They found that a biological process, termed endoplasmic reticulum stress or ER stress, is the significant driver of neuropathic pain. The research is expected to ignite the discovery of a new generation of therapeutics, paving the way for more efficient and effective ways to alleviate neuropathic pain.
Discover magazine headlined its story on the UC Davis research: “A Key Piece of the Pain Puzzle Is Solved.” Writer Heather Stringer quoted Hammock as saying: “Medications have historically focused on turning down the nerve response to pain, but now we've found one way to block the stress signal that generates the pain.

“Neuropathic pain, however, affords its sufferers no such luxuries,” Stringer pointed out. “It's chronic and unrelenting, and its cause is unknown, making treatment difficult. It turns out that neuropathic pain is triggered when the body experiences endoplasmic reticulum (ER) stress, a condition in which the production and transport of protein exceeds the cells' capacities, say researchers from the University of California, Davis. Because diabetics are at high risk of having neuropathic pain, the team studied diabetic rats that had neuropathic symptoms: hypersensitivity to touch and lack of heat sensation. And the rats' nerve cells showed clear signs of ER stress.”
“When the researchers treated the rats with a compound that blocks ER stress, the pain symptoms disappeared. Conversely, healthy rats developed neuropathy when they received chemicals that induce the stress response.”
Hammock, a member of the National Academy of Sciences and a fellow of the National Academy of Inventors, discovered a human enzyme termed sEH which regulates a new class of natural chemical mediators. He and his lab then developed inhibitors of the sEH enzyme which degrades natural mediators reducing hypertension, inflammation and pain.
The UC Davis research was earlier recommended for F1000 (Faculty 1000), a continually updated collection of more than 145,000 recommendations of top articles in biology and medicine.
The research is the work of a six-member research team: Inceoglu, Bettaieb, Haj, and Hammock, as well as K.S. Lee and Carlos Trindade da Silva, both of the Department of Entomology and Nematology and UC Davis Comprehensive Cancer Center.
Related Links:
- Discover Magazine 100 Top Stories of 2015
- Discover Magazine: Key Piece of the Pain Puzzle Is Solved
- PNAS article
- UC Davis News Story: Groundbreaking Research on Neuropathic Pain
- Faculty 1000 Honor

- Author: Kathy Keatley Garvey

The grant, “Development of an Oral Analgesic for Neuropathic Pain," is funded by the Blueprint for Neuroscience Research. National Institutes of Health (NIH).
The clinical trials, scheduled to begin in 2017, will target diabetic neuropathic pain, occurring in an estimated half of the world's 347 million diabetics, and 29 million Americans.
The compound “is an inhibitor of the soluble epoxide hydrolase (sEH) enzyme,” said Hammock, whose fundamental research on the developmental biology of insects led to the discovery. “It is a key regulatory enzyme involved in the metabolism of fatty acids and treats pain by stabilizing natural analgesic and anti-inflammatory mediators.”

“We are really honored to have been the first company to enter directly into the clinical development phase of the NIH Blueprint Neurotherapeutics Network award program,” said William Schmidt, EicOsis vice president of clinical development. “Since this was a highly competitive grant, this demonstrates the enthusiasm that the NIH has for developing non-opioid therapeutic options for treating severe pain. With the support and direct collaboration of outside experts in the NIH network, we look forward to advancing this novel type of analgesic drug into human clinical trials.”

Current therapies for diabetic neuropathy pain are ineffective in more than three of four patients. “The EicOsis technology may solve a great need in pain treatment in providing a powerful analgesic which avoids the side effects of opioids (narcotics) and nonsteroidal anti-inflammatory drugs (NSAIDs),” said physician Scott Fishman, professor and chief of the Division of Pain Medicine, UC Davis Health System, who is not affiliated with the company. “The EicOsis compound holds great promise for controlling neuropathic pain in general and particularly for this difficult and common medical problem.”
Hammock said EC5026 and close analogs have already shown to be effective “against naturally-occurring moderate-to-severe pain in dogs, cats, and horses.”

The $4 million grant will provide both financial support and shared resources for advancing the EicOsis compound through early clinical trials. The Blueprint for Neuroscience Research is a cooperative effort among the 15 NIH Institutes, centers and offices that support neuroscience research and accelerates discoveries through pooled resources and expertise.

"The Blueprint has funded early drug development efforts in the past, but EicOsis is the first group in the nation to be funded in their advanced development phase," said EicOsis project manager Cindy McReynolds, program manager of the Hammock lab in the UC Davis Department of Entomology and Nematology.
EicOsis (pronounced eye-cosis), is described on its website, http://www.eicosis.com/, as a privately held Davis-based company developing a first-in-class therapy of a once daily, oral treatment for neuropathic and inflammatory pain in humans and companion animals. Hammock developed the technology for the lead compound. UC Davis licensed the compound exclusively to EicOsis. The company maintains a strong patent position with both method-of-use and composition-of-matter patents.
Research was supported by the National Institute of Neurological Disorders and Stroke of the National Institutes of Health under Award Number UH2NS094258.
Much of the research was supported through the UC Davis Department of Entomology by the NIH, National Institute of Environmental Health Sciences (NIEHS), National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) and the American Asthma Society.
Hammock is a fellow of the National Academy of Inventors, which honors academic invention and encourages translations of inventions to benefit society. He is a member of the U.S. National Academy of Sciences, a fellow of the Entomological Society of America, and the recipient of the Bernard B. Brodie Award in Drug Metabolism, sponsored by the America Society for Pharmacology and Experimental Therapeutics. He directs the campuswide Superfund Research Program, National Institutes of Health Biotechnology Training Program, and the National Institute of Environmental Health Sciences (NIEHS) Combined Analytical Laboratory.
A member of the UC Davis faculty since 1980, Hammock received his bachelor of science degree magna cum laude from Louisiana State University in entomology and chemistry, and his doctorate from UC Berkeley in entomology and toxicology, working in xenobiotic metabolism. (For biographies on the other EicOsis officers, see website on EicOsis personnel.)
For more information, access the website at http://www.eicosis.com or contact project managere Cindy McReynolds at cbmcreynolds@eicosis.com or 530-341-4194.
Related Links:
Key mechanism that causes neuropathic pain found (July 7, 2015)
A biological process called endoplasmic reticulum stress appears to play a key role in causing neuropathic pain, according to a new study. The discovery could eventually lead to new therapeutics for controlling chronic pain associated with trauma, diabetes, shingles, multiple sclerosis or other conditions that cause nerve damage.
UC Davis to test experimental drug for laminitis in horses (VIDEO) (Nov. 14, 2012)
Veterinarians at the UC Davis School of Veterinary Medicine have announced plans to conduct the first clinical trial of an experimental drug that has shown promise in treating horses stricken with laminitis, an excruciatingly painful and often life-threatening foot-related disease.
Discovery could help combat chronic pain in diabetics (June 26, 2015)
Researchers at UC Davis have discovered a class of natural compounds found within the body that may someday lead to pain relief for millions of diabetics and others suffering from chronic pain.
Pest Control Research Leads To Pain Control Discovery (Sept. 1, 2006)
A newly discovered enzyme inhibitor, identified by researchers originally looking for biological pest controls, may lead to pain relief for sufferers of arthritis and other inflammatory diseases, say UC Davis researchers. The finding, hailed by a noted inflammatory disease expert "as the most important discovery in inflammation in more than a decade," may also reduce side effects associated with the painkiller, Vioxx.
- Author: Kathy Keatley Garvey
Embargo lifts at noon p.m. Pacific Time, July 6, 2015

DAVIS--In ground-breaking research estimated to affect millions of patients globally, scientists at the University of California, Davis have pinpointed a key mechanism that causes neuropathic pain--a complex, chronic and difficult-to-treat pain caused by nerve injuries from trauma or from such diseases as diabetes, shingles, multiple sclerosis and stroke.
A biological process, termed endoplasmic reticulum stress or ER stress, is the significant driver of neuropathic pain, said lead researchers Bora Inceoglu of the Bruce Hammock lab, UC Davis Department of Entomology and Nematology/UC Davis Comprehensive Cancer Center, and Ahmed Bettaieb of the Fawaz Haj lab, Department of Nutrition.
The ground-breaking discovery, published July 6 in the Proceedings of the National Academy of Sciences, “should ignite the discovery of a new generation of therapeutics,” paving the way for more efficient and effective ways to alleviate neuropathic pain, the researchers said.
“This is a fundamental discovery that opens new ways to control chronic pain,” said corresponding author and senior researcher Hammock, a distinguished professor of entomology who holds a joint appointment with the UC Davis Department of Entomology and Nematology, and the UC Davis Comprehensive Cancer Center.
“We can now specifically search for agents to control ER stress and its downstream pathways,” said Hammock. “This search is already underway in a number of laboratories working on cancer and other diseases.”
In the study, “Ahmed demonstrated key molecular signatures associated with diabetes and diabetic pain indicative of ER stress,” said Fawaz Haj, a senior author and corresponding author. The Haj laboratory studies the molecular basis of metabolic diseases, mainly obesity and type 2 diabetes.
“Diabetic neuropathy is a common consequence of both type 1 and type 2 diabetes which affects 60 to 70 percent of the diabetic patients,” said Ahmed Bettaieb, who has just accepted a position as assistant professor in the Department of Nutrition, University of Tennessee-Knoxville. “Knowledge on the specific contribution of individual cellular signaling pathways in the pathobiology of diabetic neuropathy is required to identify optimal drug targets. Identifying ER stress as a potential molecular mechanism that underlies diabetic neuropathic pain will open novel routes for the search of new therapeutic strategies therapies and optimizing currently available pain control medications.”
Inceoglu showed that neuropathic pain could be initiated by diverse compounds that cause ER stress and reversed by agents that block it.
"We were trying to understand how a class of natural bioactive lipids in our body can have such powerful analgesic effects,” said Inceoglu. “Our previous collaboration with Drs. Haj and Bettaieb had already established that blocking the degradation of these natural molecules is strongly analgesic (reduces pain) in diabetic animals without any of the side effects of known drugs. Expanding on these observations, in diabetic rodents, we looked at nerves and in particular those that are away from the skin, deeply embedded in the body. ER stress was obvious in these areas such as the sciatic nerve trunk and the spinal cord. Once we realized that ER stress had taken over the nervous system, we asked if it had any immediate consequences that can be measured."
Said Inceoglu: "It was an exciting moment when we could block pain in diabetic rodents using known inhibitors of ER stress. Later inducing ER stress in healthy rodents resulted in neuropathic pain-like behaviors which could be eliminated with ER stress blockers, but not so well with known drugs that are prescribed to patients suffering from neuropathic pain, with or without diabetes."
"Unfortunately, neuropathic pain remains an unmet medical need and available drugs are either not so effective or have serious side effects that limit their use in many patients,” Inceoglu said. “The bottom line is that we do not fully understand neuropathic pain and our work sheds new light onto one out of many diverse biological processes that mediate neuropathic pain. With this knowledge, one can test if ER stress blocking drugs can control pain in the clinic, and in parallel, ask fundamental questions in the lab, such as how multiple types of pain grouped under the name ‘neuropathic' differ from each other and respond to new ER stress blockers."
John Imig, professor of pharmacology and toxicology at the Medical College of Wisconsin, Milwaukee, who was not involved in the study, said: “This scientific study provides convincing evidence for a novel concept as to what causes neuropathic pain. Cellular endoplasmic reticulum stress, ER stress, has been implicated in diabetes and findings in this scientific study now implicate ER stress in neuropathic pain."
“This group of investigators previously found that drugs that target ER stress reduce symptoms of diabetes,” Imig pointed out. “Interestingly, this scientific study provides exciting data clearly demonstrating that molecular chaperones and soluble epoxide hydrolase inhibitors reduce ER stress and neuropathic pain in a synergistic manner. This provides a new opportunity for developing innovative single molecule or combination therapeutics for neuropathic pain.”
In earlier work, the UC Davis team showed that by stabilizing analgesic and anti-inflammatory natural molecules in the body, they could block ER stress and improve a variety of disease states. In this report, the researchers blocked ER stress using a powerful transition state inhibitor of the soluble epoxide hydrolase enzyme made by co-author/researcher Kin Sing Stephen Lee of the UC Davis Department of Entomology and Nematology/UC Davis Comprehensive Cancer Center.
“The compound reduces dramatically the pain associated with diabetic neuropathy and illustrates that one can reduce neuropathic pain by increasing natural chemical mediators already in the body,” said Hammock. He and his laboratory discovered and study potent enzyme inhibitors that dramatically reduce inflammation, inflammatory pain and neuropathic pain.
The research “Endoplasmic Reticulum Stress in the Peripheral Nervous System Is a Significant Driver of Neuropathic Pain,” is the work of a six-member research team: Inceoglu, Bettaieb, Lee, Haj, Hammock and Carlos Trindade da Silva of the Department of Entomology and Nematology/UC Davis Comprehensive Cancer Center.
“Despite intensive effort and resulting gains in understanding the mechanisms underlying neuropathic pain, limited success in therapeutic approaches have been attained,” the authors wrote in their abstract. “A recently identified, non-channel, nonneurotransmitter therapeutic target for pain is the enzyme soluble epoxide hydrolase (sEH).”
“The sEH degrades natural analgesic lipid mediators, epoxy fatty acids (EpFAs), therefore its inhibition stabilizes these bioactive mediators,” they explained. “Here we demonstrate the effects of EpFAs on diabetes-induced neuropathic pain and define a previously unknown mechanism of pain, regulated by endoplasmic reticulum (ER) stress. The activation of ER stress is first quantified in the peripheral nervous system of type 1 diabetic rats. We demonstrate that both pain and markers of ER stress are reversed by a chemical chaperone.”
“Next we identify the EpFAs as upstream modulation of ER stress pathways. Chemical inducers of ER stress invariable lead to pain behavior that is reversed by a chemical chaperone and an inhibitor of sEH. The rapid occurrence of pain behavior with inducers, equally rapid reversed by blockers and natural incidence of ER stress in diabetic peripheral nervous system (PNS) argue for a major role of the ER stress pathways in regulating the excitability of the nociceptive system. Understanding the role of ER stress in generation and maintenance of pain opens routes to exploit this system for therapeutic purposes.
The research was supported in part by a National Institute of Environmental Health Sciences (NIEHS) grant and a NIEHS Superfund Basic Research Program grant, awarded to principal investigator Bruce Hammock; and National Institutes of Health (NIH) grants awarded to Fawaz Haj. In addition, Hammock, Inceoglu and Bettaieb received grants from NIH and/or the National Institute of Arthritis and Musculoskeletal and Skin Disease.
Related Links
PNAS Article
Diabetes Can Be Prevented, Reversed
UC Davis Pain Research May Pave the Way to Understanding and Controlling Chronic Pain
Bruce Hammock Elected to National Academy of Inventors
Contacts:
Bruce Hammock, corresponding author
bdhammock@ucdavis.edu
(530) 752-7519 office
(530) 752-8465 message
Fawaz Haj, corresponding author
fghaj@ucdavis.edu
(530) 752-3214
Bora Inceoglu, abinceoglu@ucdavis.edu
Ahmed Bettaieb, abettaieb@ucdavis.edu

- Author: Kathy Keatley Garvey


Yes, it can--at least in genetically obese mice, according to a newly published study by researchers in the Joan Clària laboratory at the University of Barcelona, Spain, in collaboration with the Bruce Hammock laboratory of the University of California, Davis. The research involves a potent enzyme inhibitor discovered by the Hammock lab that dramatically reduces inflammation, inflammatory pain and neuropathic pain.
The groundbreaking study, published in the Proceedings of the National Academy of Sciences, involved an enzyme called soluble epoxide hydrolase (sEH) inhibitor used in mice with a high level of omega-3 fats. This treatment both prevented the onset of diabetes and reversed the effects of diabetes in obese mice.
“Our previous studies show the drug we are working on will reduce the symptoms of diabetes in mice by itself,” Hammock said, “but the excitement about Joan Clària's work is that if the mice have a genetically increased level of omega 3 fatty acids --the drug offers prevention or cure in mice.”
Worldwide, 347 million people have diabetes, according to the World Health Organization. The Center for Disease Control and Prevention (CDC) estimates that 29.1 million Americans or 9.3 percent of the population have diabetes, which is characterized by abnormal blood glucose levels. This includes 21 million diagnosed with diabetes, and 8.1 million undiagnosed.
“Epoxide metabolites of the omega 3 fatty acid DHA are stabilized by inhibiting an enzyme soluble epoxide hydrolase or sEH, and these metabolites contribute a great deal to the beneficial effects of an omega-3 diet,” Hammock explained. Previous UC Davis research in the laboratories of Bruce Hammock, Nipavan Chiamvimonvat, Robert Weiss, Anne Knowlton and Fawaz Haj showed that the enzyme reduces or reverses such diabetes-linked medical issues as renal failure, hypertension, diabetic pain, hardening of the arteries, and heart failure.
“This exciting research brings mechanistic detail to understanding how omega-3 fatty acids in the diet exert important health effects,” said UC Davis Professor J. Bruce German, director of the Foods for Health Institute, Department of Food Science and Technology, who was not involved in the diabetes-based research. “Such breakthroughs catalyze both research and practical health applications.”
The Joan Clària lab in Barcelona led the eight-member team study. Clària is an associate professor at the Barcelona University School of Medicine and a senior consultant at the Biochemistry and Molecular Genetics Service of the Hospital Clínic of Barcelona.
In the paper, titled “Inhibition of Soluble Epoxide Hydrolase Modulates Inflammation and Autophagy in Obese Adipose Tissue and Liver: Role for Omega-3 Epoxides,” Clària described the administration of the sEH inhibitor as “a promising strategy to prevent obesity-related co-morbidities.” He said the study “demonstrates that stabilization of cytochrome P-450 epoxides derived from omega-3 polyunsaturated fatty acids through inhibition of the inactivating enzyme soluble epoxide hydrolase (sEH) exerts beneficial actions in counteracting metabolic disorders associated with obesity, including insulin resistance and fatty liver disease.”

In addition to Clària and Hammock, the publication was first-authored by Cristina López-Vicario and co-authored by José Alcaraz-Quiles, Verónica García-Alonso, Bibiana Rius, Aritz Lopategi, Ester Titos and Vicente Arroyo, all of the Clària lab or associates; and Sung Hee Hwang of the Hammock Lab, UC Davis Department of Entomology and Nematology and the UC Davis Comprehensive Cancer Center
Clària's primary research focuses on the study of inflammatory lipid mediators involved in the development of adipose tissue inflammation and its impact on metabolic complications associated with obesity. His laboratory is centered in exploring the role of bioactive lipid mediators generated from omega-3 polyunsaturated fatty acids, especially those with anti-inflammatory and pro-resolution properties. His work places major emphasis on prevailing obesity associated hepatic co-morbidities, especially on non-alcoholic fatty liver disease.
Hammock, who holds a joint appointment with the UC Davis Department of Entomology and Nematology and the UC Davis Comprehensive Cancer Center, has worked on the mechanism of hydrolytic enzymes and their effect on human health for more than 35 years. He is developing both enzyme inhibitors and natural products as drugs for use in the United States and developing countries. His work has helped identify new targets for the action of drugs and other compounds to improve health and predict risk from various environmental chemicals.
Hammock is the founder and CEO of EicOsis, and through EicOsis, the compounds are in clinical trials for companion animals and the Pre-Investigational New Drug Application (Pre-IND) Consultation Program for neuropathic pain in human diabetics.
Hammock was recently selected a fellow of the National Academy of Inventors (NAI), which honors academic invention and encourages translations of inventions to benefit society and a member of the National Academy of Sciences. He directs the campuswide Superfund Research Program and National Institutes of Health Biotechnology Training Program.
The study was funded by Clària's Spanish-initiated grants and by Hammock's Research Project Grant (R01) and Superfund grants from the National Institutes of Health.
Links:
Bruce Hammock lab
http://www.biopestlab.ucdavis.edu/
Email: bdhammock@ucdavis.edu
Joan Clària lab
http://cdb.hospitalclinic.org/facultativos/38/joan-claria-enrich
Email: JCLARIA@clinic.ub.es
PNAS Paper
http://www.pnas.org/content/early/2014/12/30/1422590112.abstract



