- Author: Devii R. Rao

- Author: Devii R. Rao
Last week the Backcountry Horsemen of California had their Rendezvous at the Paso Robles Event Center. It was a wonderful event with great people and fun activities. In case you missed my talk on toxic plants and forage value of grasses, here's my presentation along with a few other useful resources for horse owners.
- PowerPoint presentation on toxic plants and forage value of grasses
- Livestock Poisoning Plants of California
- Field Guide for Common California Rangeland and Pasture Plants
- Establishing and Managing Irrigated Pasture for Horses
Feel free to get in touch with me (drorao@ucanr.edu or 831-637-5346 x14) if you have any questions.
BackcountryHorsemen
- Author: Devii R. Rao
Are you a rancher who is frustrated with computers? Join us on May 17 to learn some fun and easy ways to use computers and mobile devices to improve your business.
Date: Thursday, May 17, 2018
Time: 8:00 am to 11:00 am
Location: Hollister Veteran's Memorial Building, 649 San Benito St, Hollister, CA
Cost: $10. Registration includes coffee, light snacks, and handouts.
Register here: https://ucanr.edu/survey/survey.cfm?surveynumber=24635 or contact Devii Rao at drorao@ucanr.edu or 831-637-5346 x14. Registration deadline is May 11.
Join us to learn about the following topics:
- Computer hardware
- Computer operating systems
- Smartphones, tablets, and Chrome
- Cloud computing
- Online economic tools for ranchers
- Smartphone apps for ranchers
Special guest Smittie Smith, owner of RanchHacks, is a Montana-based technology consultant with a particular interest in technology applications in ranching and livestock production. From basic business information systems infrastructure to industry specifics like herd and pasture management, he educates and trains commercial and seed stock operators to leverage technology: http://ranchhacks.com.
UCCE Wesbiste: http://cesanbenito.ucanr.edu/livestock/
ComputersForCattlemen Flyer
- Author: Devii R. Rao

In the past, selenium deficiencies were common in places like Oregon, but due to extensive selenium supplementation throughout the state, WMD and other selenium deficiency disorders are now infrequent6. In California, on the other hand, selenium deficiencies continue to be an important health risk to livestock in more than 60% of the state's herds7. This article will focus on WMD caused by selenium deficiency in California beef cattle.
WMD can affect cardiac, respiratory, and skeletal muscle tissue4. Cattle whose cardiac muscles are affected can have respiratory problems, cardiac arrhythmias, or can die. Respiratory problems can also manifest in animals whose respiratory muscles are affected. Those with WMD affecting their skeletal muscles may experience stiffness, and weak damaged muscles, particularly in their hind legs, making it difficult to stand or nurse4,8,9. As the muscle degeneration occurs, calcium salts are incorporated into striated muscle fibers causing whitish lines, which is where the name white muscle disease comes from3,9. Treatment of cattle with cardiac WMD is ineffective and animals usually die in less than 24 hours4. These animals are typically between a few days to a few weeks old8. Treatment for animals with skeletal WMD, on the other hand, can be effective and improve their condition in 3-5 days4.
Calves born from cows that have adequate selenium will themselves have adequate stores of selenium for 30-60 days after they are born8. However, calves will not able to effectively obtain selenium from their mother's milk. One study showed that nursing calves, without access to supplemental selenium, became either low or deficient in selenium, even when their mothers were provided with optimal amounts of selenium10. The one exception was cows supplemented with an organic form of selenium (selenium-yeast) through a free-choice mineral mix. Organic mineral forms are known to have high rates of absorption and are effective at circulating minerals throughout the blood stream8.
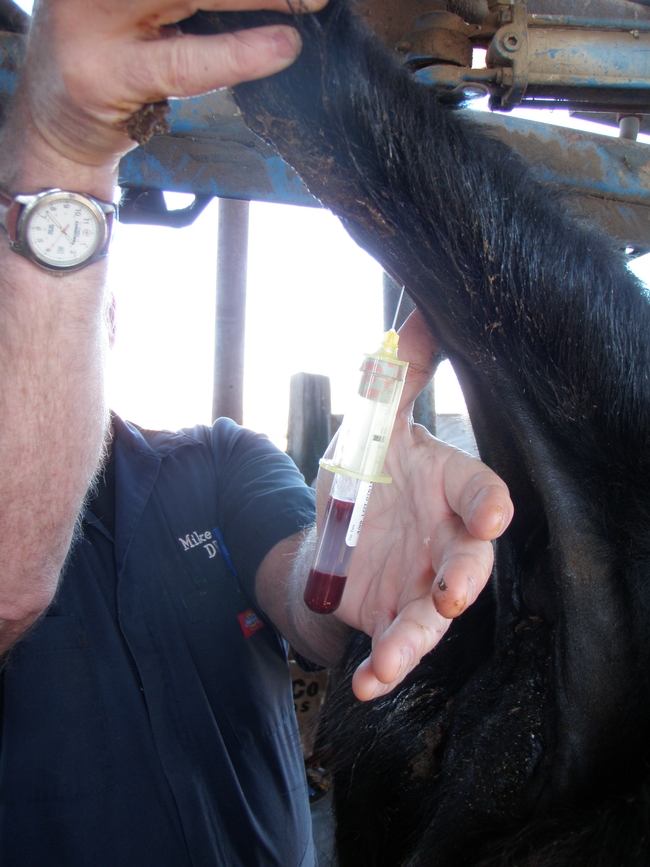
In order to prevent WMD and other selenium deficiency disorders, cattle can be given selenium supplements that can be injected, or provided through mineral mixes or a bolus5 (Figures 2 and 3). The bolus is only legal in California11. Supplementing pregnant or lactating cows and newborn calves is particularly important in order to avoid WMD3. Selenium also has the potential to be toxic and is therefore regulated by the U.S. Food and Drug Administration. The maximum allowed by law in a salt mix is 3 mg of selenium (about 1 ounce of salt mix) per animal per day2. This is the recommended amount. Selenium supplementation can come in 2 forms: inorganic or organic11. Inorganic selenium can be provided as sodium selenite or sodium selenate salts. Sodium selenite is the more commonly used because it is readily available. Selenomethionine is the organic form of selenium and is able to integrate into muscle tissue. Because of this, it remains in the body of ruminants substantially longer than inorganic forms of selenium. Thankfully, WMD is a disease that can be treated. Many California livestock producers will improve cattle health and profits if they are able to implement an effective selenium supplementation program.


CITATIONS
1CAHFS Laboratory System Annual Report 2000. 2001. School of Veterinary Medicine, UC Davis. pp. 24 25.
2Maas, J. 1998. Trace Minerals for Cattle: An Update. UC Davis Vet Views, California Cattlemen, November 1998. http://ucanr.edu/sites/UCCE_LR/files/151748.pdf, last accessed 7/31/2016.
3Pond, W.G., D.C. Church, K.R. Pond, and P.A. Schoknecht. 2005. Basic Animal Nutrition and Feeding, 5th edition, John Wiley & Sons Inc., New York.
4Valberg, S.J. 2014. Nutritional Myopathies in Ruminants and Pigs. The Merck Veterinary Manual. Last full review/revision April 2014 by Stephanie J. Valberg, DVM, PhD, DACVIM, ACVSMR. http://bit.ly/2aCX1vl, last accessed 7/31/2016.
5Forero, L., Drake, D., Nader, G. 2008. Summary of Selenium, Copper and Zinc Status for Beef Cattle in Northern California. Northern California Ranch Update. Volume 2. Issue 1. http://bit.ly/2aa2mu0, last accessed 7/31/2016.
6Oldfield, J.E., 1989. Selenium in animal nutrition: the Oregon and San Joaquin Valley (California) experiences—examples of correctable deficiencies in livestock. Biological trace element research, 20(1-2), pp.23-29. http://www.ncbi.nlm.nih.gov/pubmed/2484399, last accessed 7/31/2016.
7Dunbar, J. R, B. B. Norman, and M. N. Oliver. 1988. Preliminary report on the survey of selenium whole blood values of beef herds in twelve central and coastal California counties. Pages 81-83. Selenium contents in animal and human food crops grown in California. Cooperative Extension, University of California Division of Agriculture and Natural Resources, Publication 3330. Oakland, California.
8Hall, J.B. 2006. Selenium Supplementation Strategies for Cow/Calf Herds. The Cow-Calf Manager Newsletter. April 2006. Virginia Cooperative Extension. Virginia Tech, Virginia State University. http://www.sites.ext.vt.edu/newsletter-archive/livestock/aps-06_04/aps-313.html, last accessed 8/3/2016.
9Hansen, D., R. Hathaway, and J.E. Oldfield. 1993. White muscle and other selenium-responsive diseases of livestock. PNW 157. Revised May 1993. http://www.multiminusa.com/sites/www.multiminusa.com/files/pdfs/se_responsive_diseases.pdf, last accessed 8/3/2016.
10Davis P.A., L.R. McDowell, R. Van Alstyne, T.T. Marshall, C.D. Buergelt, R.N. Weldon, and N.S. Wilkinson. 2005. Case Study: Tissue and Blood Selenium Concentrations and Performance of Beef Calves from Dams Receiving Different Forms of Selenium Supplementation. Prof. Anim. Sci. 21:486-494.
11Brummer, F.A., G.J. Pirelli, and J. A. Hall. 2014. Selenium Supplementation Strategies for Livestock in Oregon. Oregon State University Extension Service. http://bit.ly/2aUBU4P, last accessed 7/31/2016.
12Davy, J. 2015. Livestock, Range, and Natural Resources Advisor, University of California Cooperative Extension, personal communication.
- Author: Matthew Shapero
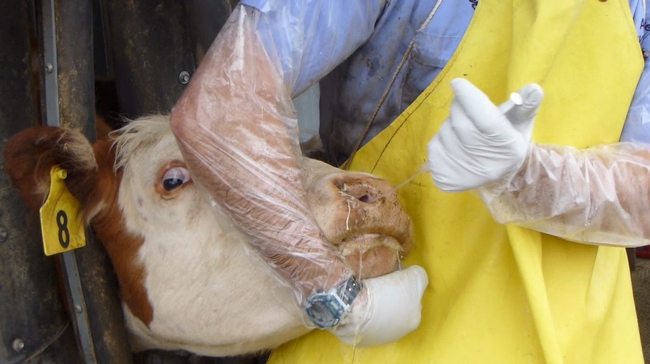
(this article is adapted from an article by the UC Davis School of Veterinary Medicine and is based on the work of John Angelos, DVM, PhD; Dr. Angelos provided additional editing)
Pinkeye—or infectious bovine keratoconjunctivitis—is the most common eye disease of cattle in California and throughout the U.S. Pinkeye causes pain and suffering in affected animals that negatively impacts overall animal welfare as well as economic losses to cattle producers. One 2005 study showed, for example, that calves that had previously had pinkeye were on average 20 pounds lighter than unaffected animals at weaning. And another, earlier study showed that bull calves one- year post-weaning were 51 pounds lighter if they had had pinkeye in one eye and 103 pounds lighter if they had had it in two eyes. These studies emphasize that prevention is of the utmost importance.
Pinkeye is caused by infection of the cornea with Moraxella bovis (M. bovis) bacteria and results in painful corneal ulcers and inflammation of the eye and skin surfaces lining the eye (conjunctiva). If not properly treated, corneal infections can result in corneal scars or even eyeball ruptures leading to permanent blindness. Another bacterium that has been associated with pinkeye, but which has not been experimentally shown to cause corneal ulcerations typical of pinkeye is Moraxella bovoculi (M. bovoculi). Currently there are vaccines on the market against both M. bovis and M. bovoculi (see below).
Pinkeye is most common in the summer months with increased exposure to sunlight and dry, dusty conditions. Some outbreaks also occur during winter months. Plant awns such as foxtails can also predispose animals to disease by getting caught in the eye and damaging the cornea. Flies also increase the chances of exposure and spread of M. bovis (and probably M. bovoculi) bacteria by feeding around the face and eyes of affected cattle and then transferring infected eye fluids to other animals. Humans might also help spread the disease particularly when they are not wearing disposable gloves or applying disinfectants to halters or other objects involved in handling affected animals.
Common signs of pinkeye:
-
Excessive tearing
-
Frequent blinking or squinting
-
Decreased appetite due to eye pain
-
Corneal ulceration and cloudiness
-
Potential blindness or eye rupture
-
Can affect one or both eyes
- Younger cattle typically more susceptible
Prevention:
Fly control: Controlling flies should help to reduce the risks of disease spread between animals in a herd. Traditional methods have included the use of insecticide-containing ear tags, dust bags, and systemically- or topically-applied parasiticides. A 1990s study looked at four different fly control strategies: 1) Ivermectin pour-on (0.5% pour-on @ 500ug/kg); 2) insecticide ear tags with permethrin (10%); 3) insecticide ear tags with diazinon (20%); and 4) Ivermectin plus ear tag in mid- summer. The best face fly control was the permethrin ear tags alone or in combination with Ivermectin (but not Ivermectin alone). Consider applying insecticide ear tags in the late spring/summer at preg-checking time. It is also a good practice to remove ear tags at the end of the fly season to help reduce chances for insecticide resistant fly populations to develop.
Weed control: Since foxtails and other plant awns can lead to corneal ulceration and eventual pinkeye, one recommendation is to clip pastures that have already seeded out before turning cattle onto that pasture.
Practice good sanitation/hygiene: To avoid inadvertently spreading infective bacteria between animals, use disposable gloves when handling pinkeye-affected cattle. These gloves should be changed or at least disinfected between animals. In addition, consider changing clothes or wearing a plastic apron when handling affected animals. It is a good practice to also disinfect plastic aprons and halters between cattle. One commonly used disinfectant is 10% household bleach made by mixing one part of regular strength household bleach to nine parts water (or ~1-1.5 cups regular strength bleach per gallon of clean water). If using concentrated bleach you will only need ~1/2 cup per gallon of clean water. This mixture should be made fresh daily to maintain effectiveness. Also, bleach becomes less effective when it becomes heavily soiled with dirt or manure and other organic material. For that reason it may need to be refreshed more frequently, depending on use and working conditions.
Trace minerals: Some trace mineral deficiencies in cattle have been linked to reduced immune responsiveness and might also lead to elevated rates of pinkeye. When it comes to pinkeye prevention, maintaining adequate levels of copper and selenium is particularly important in this part of the country. Other trace minerals/vitamins which may be important for maintaining optimum immune responsiveness and therefore might impact pinkeye prevalence include chromium, Vitamin A, Beta-carotene, cobalt, and zinc. This is yet another reason to make sure you have a robust trace mineral supplementation program on your ranch!
Vaccinate: Vaccination is another important component of pinkeye prevention, however, even with vaccination, producers may still experience pinkeye problems with today's vaccines. When vaccinating animals, it is important to vaccinate well in advance (ideally start the vaccine series at least four weeks) of the anticipated summer onset of pinkeye in your herd, so that cattle will have enough time to mount an effective immune response following vaccination. Depending on the vaccine used, a booster shot 3-4 weeks following the initial vaccine may also be required by the manufacturer; it is a good idea to follow vaccine manufacturer recommendations regarding booster vaccines. Because young animals tend to be most affected, it is critical that they are included in the vaccination program. No single vaccine recommendations work for all herds. If you have not used a pinkeye vaccine before, a reasonable approach is to start by choosing a commercial M. bovis vaccine. If your initial vaccine choice proves ineffective, a variety of options exist including: 1) a different commercial product; 2) an autogenous vaccine, based on eye swabs from infected animals you send in to the lab; or 3) perhaps both. The newest product available on the market (as of 3/2/17) is a Moraxella Bovoculi bacterin from the Addison Biological Laboratory. Dr. Angelos at UC Davis School of Veterinary Medicine has been developing an intranasal pinkeye vaccine that might provide better eye immune responses versus traditional subcutaneously injected vaccines.
Dr. John Angelos administers an experimental intranasal pinkeye vaccination at the UC Sierra Foothill Research and Extension Center.
Treatment:
Pinkeye is susceptible to a wide variety of antibiotics; however only two are specifically labelled for the treatment of pinkeye: tulathromycin and oxytetracycline. Other antibiotics are known to be effective, but the use of these drugs for pinkeye treatment is considered “off-label.” Using one of these other drugs should be done under the supervision of your veterinarian. An effective non- antibiotic treatment that might be worth considering is Vetericyn pinkeye spray. Research shows that Vetericyn reduced pain, infection, and healing time of corneal lesions in calves infected with pinkeye. While other treatments such as salt, condensed milk, and dilute povidone iodine have been used by producers, research has not been done on these types of treatments to determine if they are truly effective against pinkeye. Before squirting something in the affected cow or calf's eye, it is always a good idea to ask yourself if you would want that material squirted in your own eye. If your answer is ‘no', it is probably best not to put it in an animal's eye. If ever in doubt, it is always a good idea to consult with your veterinarian for specific treatment recommendations.
Perhaps one of the most difficult aspects of pinkeye treatment is knowing when it is appropriate to use antibiotics. In many instances, eyes that may look like mild or developing pinkeye will heal spontaneously when given time. If you are able to hold the animal for a period of 7-14 days and regularly check the eye, you may choose to withhold antibiotics initially from the animal in order to monitor the eye's progress. This is especially true for animals that have a foreign body (e.g. foxtail) in their eye, which can scratch and irritate the corneal surface around the perimeter of the cornea. Once the foxtail is removed, however, the eye will frequently heal on its own and will not become infected. In many production settings, however, holding an animal for multiple days and/or regularly restraining the animal to inspect the eye is unrealistic, thus an application of antibiotics upon initial identification is appropriate.
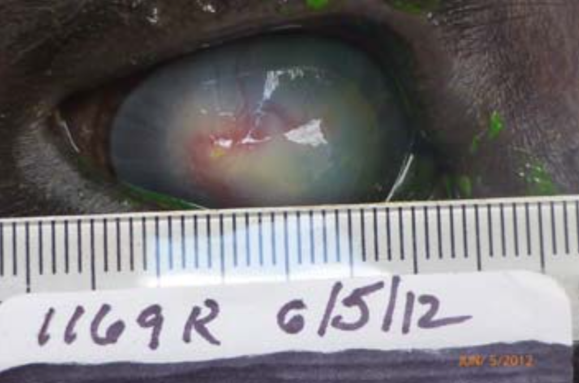
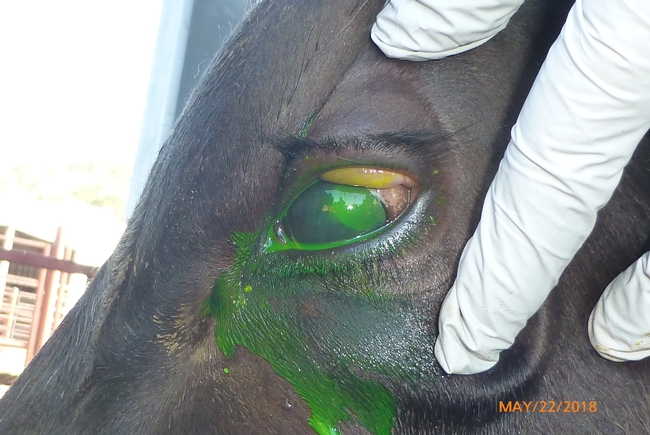
You may also encounter eyes that look like a developing pinkeye, when really they have already begun the healing process. Consider Figure 1, which shows an eye from the same cow on 5/22/12 and 6/5/12. This animal was not treated with antibiotics. The green color is fluorescein, which is a dye that is added to the eye to better identify corneal ulcers associated with pinkeye. On 5/22/12 the animal showed a typical ulcer (area in green); by 6/5/12 the eye had begun to heal. If you came across this animal on 6/5/12 on the ranch, however, you wouldn't have the benefit of knowing the trajectory of the eye's healing process. While antibiotics would not be necessary, it would be difficult to know not to apply them. One important indication that the eye is already healing (and thus does not require antibiotics) is the presence of red blood vessels covering the cloudy part of the eye (see 6/5/12 photo from Figure 1). Other indications that an eye is well on its way to healing and may not need antibiotics is if the eye is not excessively teary or weeping and if the animal is not actively squinting or sensitive to light.
Figure 1.
Some producers will apply an eye patch to a pinkeye-affected eye after they have treated the animal. Using old jeans and tag cement is common. Patches likely provide some comfort to the animal, as it protects the eye from sunlight and potentially dust and flies. Make sure to leave the patch open at the bottom for drainage and air circulation. One important point with patches, however, is that eyes should be checked regularly after applying a patch. Just because you can't see the eye when it's covered by the patch, doesn't mean the eye is doing well. Therefore, make sure you check under the patch frequently to know if the eye is healing or not; checking under a patch ideally a couple of times during the first week after putting it on will help you to know if the eye is improving or not.
All treatment programs should be overseen by your herd veterinarian who can assess the situation and recommend the best prevention and treatment protocol.
Eye stained with fluorescein after removing foxtail. Note ulcer (highlighted in green) on the right edge of the eyeball. Ulcers caused by foxtails or other foreign objects will present on the perimeter of the cornea. This eye healed without the use of antibiotics.