Posts Tagged: Patricia Crawford
Children are getting healthier, but the obesity crisis is not over
Real progress has been made in tackling the epidemic of childhood obesity since the first California Childhood Obesity Conference was held 20 years ago, but there is more work to be done.
“Collectively, we have come so far,” UC Nutrition Policy Institute Director Lorrene Ritchie told an audience of 1,025 public health, nutrition education, research, and other professionals at the event in Anaheim in July 2019. NPI was one of six conference hosts.
In the last 20 years:
- Federal school meal standards have been revised so that the food children eat at school is healthier than the lunches they bring from home.
- Sugar-sweetened beverages are no longer available to students during the school day.
- Foods provided by the Special Supplemental Nutrition Program for Women, Infants and Children (WIC) are healthier and give mothers incentive to breast feed their babies.
- The Supplemental Nutrition Assistance Program (SNAP) education component is now linked to policy, systems and environmental changes.
- The Child and Adult Care Food Program now provides healthier meals and snacks to children in childcare centers and homes across the country.
The average quality of the diet of American children has improved, but the rate of childhood obesity in the United States is still too high.
According to the Centers for Disease Control and Prevention, 18.5% of U.S. children and adolescents 2 to 19 years old are obese – about 13.7 million youth in all. The rates trend higher in minority communities, with 25.8% of Latinx youth and 22% of African American youth obese. Obesity is also more prevalent among children in families with low incomes.
Obesity, which is defined in children as a body mass index at or above the 95th percentile of CDC growth charts, is associated with poorer mental health status, reduced quality of life, and increased prevalence of diabetes, heart disease, stroke and some types of cancer.

The vice president of UC Agriculture and Natural Resources, Glenda Humiston, pledged the organization's commitment to community health and wellbeing at the Childhood Obesity Conference. UC ANR is the umbrella organization of the Nutrition Policy Institute, UC CalFresh Healthy Living, UC Cooperative Extension, 4-H Youth Development, the UC Master Gardener Program and the California Naturalist Program, among others.
“Going forward, solutions to the obesity epidemic are multidisciplinary,” Humiston said. “NPI does world class work in conducting research to influence nutrition policy. We need to harness 4-H. Master Gardeners are increasingly focusing on edible gardens. CalNat is getting people out into nature. We are finding synergies in community wellness.”
Humiston has dedicated UC ANR resources to finding and implementing solutions to the obesity crisis.
“I'm looking forward to working with all of you – public and private organizations – to design a way to move forward,” she said.
The opening keynote presentation at the conference featured Patricia Crawford, NPI's Senior Director of Research emeritus, a pioneer in addressing the growing problem of childhood obesity during her long career. Beginning in the 1970s, she recognized that childhood obesity was on the rise and launched several studies to search for the causes and potential solutions.
In one study, Crawford followed a group of 9-year-old African American girls over a period of 10 years to determine why these youth were growing up heavier than other adolescents.
“Finally, we began to get some answers,” Crawford said. “We learned obesity wasn't the children's fault. They were living in environments that made the unhealthy choice cheaper and easier to find. It's so unfair for people who have fewer resources. Health disparities has to be the No. 1 thing we are working on to address chronic disease rates in this country.”
“The solution to obesity is prevention. It's cheaper and more effective than treatment,” Crawford continued. “Healthy food is a taste that is easy to acquire if it is not preempted by junk food.”
Crawford said she honed in on the best strategies for prevention by actively listening to people struggling to make healthy choices
“There is a chasm between research and community,” Crawford said. “We have to get people together from the research level and the policy level with folks on the ground. We need to learn from people.”
Catalyst of change Pat Crawford’s research helps advance food policies

The San Francisco Chronicle reported this exercise in a 2016 interview with Crawford about newly approved USDA nutrition labels that would include added sugar information and thereby eliminate the need for such complex computations by consumers. Sadly, these nutrition guidelines have yet to come out. Why not, if we know that added sugar is related to heart disease, diabetes, tooth decay and other negative health conditions? Why hasn't this regulation been adopted? Crawford works to provide the research needed by policymakers to reduce the barriers to implementation of helpful policies such as this one.
Pat Crawford's work on improved food labeling is but one example of the way that for decades her timely and rigorous research has demonstrated the role of sugary foods and beverages in the development of diabetes, and obesity and in helping to fuel America's childhood obesity epidemic. In countless ways Crawford, who is retiring this year after more than 40 years of service at the University of California, has supported the adoption of public policies that promote safer, healthier food and beverages for all people, across the state and the nation.
You can draw direct lines from her resume to countless major policy advances in nutrition education and public health. Since earning her master's degree in public health nutrition and her registered dietician credential at UC Berkeley in 1972, Crawford has been a force of unceasing productivity as a researcher, an evaluator, an educator and a leader. Early in her career she managed the nation's largest biracial study of girls' health, the National Growth and Health Study. During the course of this long-term study, she went back to school to obtain her doctorate in public health nutrition. She soon was hired as the first UC Cooperative Extension Nutrition and Obesity Prevention specialist and she co-founded and directed UC Berkeley's Atkins Center for Weight and Health. The work of the center focused largely on food and nutrition policy to improve the health of children, and it provided a structure whereby University research could be effectively shared with community health workers throughout the state. Local and state health professionals found in the center an extension partner eager to conduct research that would answer important questions and provide real-world solutions, productively linking research, policy and practice.
The Center for Weight and Health, which in 2015 merged with the UC ANR Nutrition Policy Institute (NPI), became known for rigorous research that is aligned with UC ANR's core values of addressing food security, obesity, socioeconomically based health disparities, and access to healthy foods. After the merger, Crawford became NPI's Senior Director of Research, working with her long time collaborator, Lorrene Ritchie, the NPI director.
Ritchie stated that in addition to Crawford's academic achievements, she is the consummate mentor — a “career godmother” for Ritchie and many others. She said, “Pat has an uncanny ability of knowing what you are good at — even before you yourself do — and mentoring you to build on that strength. Likewise, she has an uncanny ability to know your weaknesses, and help you to overcome those by developing new skills or pairing you with others who have those skills.”
That kind of nurturing is rare, Ritchie noted, particularly in the competitive environment of academia. Through mentoring, she added, Crawford has ensured new generations of researchers will continue this work.
“Pat has proven that you can be caring and compassionate yet still be highly effective.”
Catalyzing change
What does highly effective look like? A few examples illustrate the impact that Pat Crawford's work has had on nutrition policies and trends.
To improve the food environment at child care centers and schools, the Center/NPI provided the evidence for:
- California's 2010 Healthy Beverages in Childcare Law, requiring child care centers to make water and other healthy beverages available at all times.
- The 2013 Foundations for Healthy Nutrition in Childcare Act, requiring nutrition education for all child care providers.
- “Competitive food” policies — banning unhealthy sodas and snacks that competed with more nutritious school lunches — a policy that started in California and later was implemented at the federal level in the USDA's 2016 “Smart Snacks Standards.”
- The expansion of school garden and cooking programs in California and nationwide.
- An expansion of support for replacing packaged foods with healthier scratch cooking in school cafeterias.
To promote more nutritious food in programs serving low-income families the Center/NPI advocated:
- Improvements in the federal Women, Infants and Children (WIC) program including quadrupling the amount of vegetables and legumes WIC provides and adding information about physical activity needs for young children.
- Food bank policies that increase the amount of fruits and vegetables distributed and reduce the amount of snack foods and sugary beverages. Their free online course on how to make these policy shifts is a popular web resource for food banks across the country.
To advance education and communication:
- Crawford co-founded the first interdisciplinary conference on childhood obesity. Twenty years later, the biennial meeting is the premier obesity conference in the nation.
- The “My Healthy Plate” nutrition-education tool, which replaced the old Healthy Eating Pyramid, was developed, tested, presented and promoted by Crawford and her extension colleagues before the plate concept was officially adopted by USDA in 2011.
- California became the first state to put calories on chain-restaurant menus. Crawford's evaluation of Kaiser Permanente's pilot study of menu-board labeling provided the evidence needed by policymakers. Calorie labeling in chain restaurants has been expanded nationwide.
- Crawford's evaluation of California's SNAP-Ed program, the education arm of the Supplemental Nutrition Assistance Program, (or SNAP, previously known as food stamps), has informed programming focused on the prevention of chronic disease through efficacious nutrition changes in the environment.
Although Crawford would be quick to tell you that her work is collaborative, she has been a researcher or important influence on nearly every population-based nutrition policy success. She has served as president of the California Nutrition Council and on countless state and national committees and task forces focused on improving health and addressing obesity, including being an advisor to California's Let's Get Healthy Task Force. Most recently, she co-authored a seminal Healthy People 2020 report for the U.S. Department of Health and Human Services, Office of Disease Prevention and Health Promotion, on model policies to increase fruit and vegetable intake in the population.
Training the next generation
Given her commitment and her influence, it's no wonder that Pat Crawford won the 2013 David Kessler Award for Extraordinary Contributions to the Public's Health, as well as multiple honors from the American Public Health Association. In 2018, the UC Berkeley School of Public Health honored Crawford as one of its 75 most influential alumni in recognition of her significant contributions to reduce the epidemic of childhood obesity in California and across the country. And she's not done yet — as an emeritus Cooperative Extension specialist, her research will go on. That won't surprise anyone who knows her. As Crawford said in a 2015 interview, “What keeps me passionate is knowing that change is possible when high-quality, policy-relevant research is conducted and communicated to decision-makers and those who work with children.”
To honor the work that Crawford does and to continue this kind of work, the Nutrition Policy Institute has established a student fellowship fund to train the next generation of students on nutrition research and its policy impacts. Donors to the student fellowship fund help honor Crawford and help NPI continue its work to improve the nutrition and health of children.
UC's Pat Crawford weighs in on childhood obesity

So today seems the perfect time to revisit a 2015 conversation with Rose Hayden-Smith, UC's Food Observer, and Crawford, now the Senior Director of Research at UC ANR's Nutrition Policy Institute. As Pat stated in her interview—
“Not changing is risky. The United States – along with Mexico – has the highest obesity rates in the industrialized world. With these extraordinarily high obesity rates, we are on a path toward ever-rising chronic disease rates including not just diabetes, but also heart disease and some cancers, increasing health care costs and reducing productivity.
Even more alarming, is a little known fact that 23 percent of the adolescents in this country currently have pre-diabetes or diabetes as measured by actual blood tests in our largest national study of health (NHANES). Something is seriously wrong in a society such as ours where so many children are growing up with such a high risk of preventable disease.”
You can read the complete interview at the UC Food Observer. You'll also find a recent story about the 45 youth advocates from organizations around California joining this year's conference to bring the voices of youth to this vital conversation.
Beverage industry using defensive tactics to fight soda tax initiatives
The beverage industry is recruiting low-income and minority groups to help share a message aimed at tanking soda-tax measures in Oakland and San Francisco, reported Winston Cho in the East Bay Express.
The industry has poured in $13 million to fight Oakland's Measure HH and San Francisco's Proposition V, the story said. The groups supporting the measures have received contributions of nearly $4 million, making Measure HH one of Oakland's best-funded initiatives ever.
The American Beverage Association is positioning the tax measures as "grocery taxes," saying that low-income consumers will bear the brunt.
"I think the money invested, in addition to the framing — which is specifically not mentioning sugary beverages — suggests that there's a lot of defense in their offense," said Wendi Gosliner, policy researcher at the UC Nutrition Policy Institute.
The Nutrition Policy Institute is a UC Agriculture and Natural Resources program that conducts and evaluates research related to the impact of nutrition and physical activity on public health.
Patricia Crawford, senior director of research at the Nutrition Policy Institute, told the reporter that justifying the soda tax to the low-income community in Berkeley was an essential part of getting it passed in that community two years ago. NPI hosted multiple town halls when that tax was on the ballot. They invited professors, doctors, and health-care professionals to address the community's concerns.
"People think of soda as just another candy or food, and it isn't," Crawford said. "[The negative impact on public health] is just too costly ... for us to ignore."
In an article Crawford wrote for the UC Food Blog, she reflected on recent research that showed the Berkeley soda tax successfully reduced consumption of sugar-sweetened beverages while raising funds to promote health and wellness activities in Berkeley schools.
"The Bay Area has long been an early adopter of many important ideas, initiating movements that have spread across the country. Will Oakland, Albany and San Francisco follow Berkeley's lead to a healthier future for their communities?" Crawford wrote.

UC CalFresh nutrition educator Nancy Zumkeller shows the amount of sugar in a 32-ounce soda.
As Americans struggle with obesity and diabetes, help is on the way

The decision, reflecting the latest science, will be felt well beyond the label. University of California food experts praised the labeling changes and offered six key takeaways.
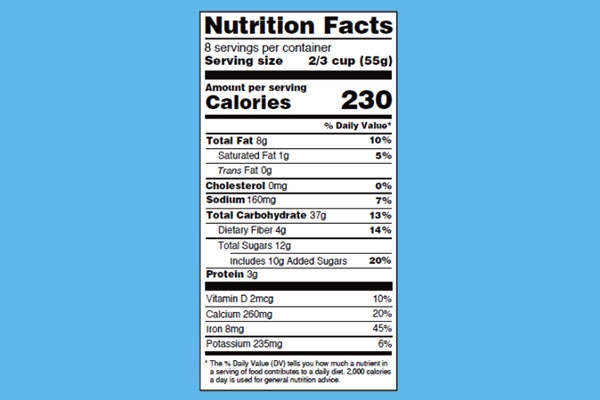
1. Listing added sugar is the most important label change.
The new label will list the amount of added sugar in a product, both in grams and as a percentage of the daily recommended allowance.
“That's key,” said Laura Schmidt, a UC San Francisco professor of health policy and UC Global Food Initiative subcommittee member. “That will be really helpful for consumers.”
Added sugar – any sugar added in the preparation of foods such as table sugar, high fructose corn syrup and others – can be found in hundreds of products such as cereal, yogurt, pasta sauce and salad dressing. But the biggest source is sugar-sweetened beverages, which account for nearly half of Americans' intake of added sugar.
One 20-ounce soda will take you over the recommended amount of sugar for an entire day,” said Pat Crawford, senior director of research for the Nutrition Policy Institute of UC's Division of Agriculture and Natural Resources. “The new label will allow people to reasonably see what they're doing when they're consuming high-sugar products.”
The current label lumps added sugar with naturally occurring sugars in the foods themselves, which is a deceptive practice, said Dr. John Swartzberg, a UC Berkeley clinical professor emeritus and editorial board chair of the UC Berkeley Wellness Letter. Listing added sugar “will hopefully guide people away from consuming products with a lot of added sugar,” he said.

More than one out of three adults in the U.S. is obese. Nearly half of U.S. adults have prediabetes or diabetes, raising their risk of heart attacks, kidney failure, blindness and amputations. Among U.S. children, more than 1 in 6 is obese, and diabetes and prediabetes rates are rising. Amid these alarming statistics, there's a growing concern about too much added sugar in diets.
“It's important to give the public the information they need in order to modify their diets,” Crawford said. “We are now finding significant effects on diabetes and heart disease rates for those who regularly consume sugary beverages. A large study of women over an eight-year period found that the risk of diabetes among women who consumed one or more servings of sugar-sweetened beverages per day was nearly double the risk among women who consumed less than one serving per month. Further, drinking one 12-ounce soda a day increases the risk of cardiovascular mortality by almost one-third.”
Crawford noted that the new federal dietary guidelines for the first time recommend limiting added sugars in the diet to no more than 10 percent of one's daily calories.
“The average amount of added sugar in the American diet is more than 20 teaspoons per day, nearly all of which is added to our foods during processing,” Crawford said. “Since about half of this sugar comes in the form of beverages, we have to rethink our beverage choices. Water should be the beverage of choice.”
Consumers will be very surprised to see the percentage of daily value of added sugar in one soda drink, said Michael Roberts, executive director of the UCLA Resnick Program for Food Law and Policy and UC Global Food Initiative subcommittee member. “Time will tell whether this information changes human behavior, i.e., consuming less soda. To be fair, sugar pops up everywhere, not just soda, so the impact that these changes will have on consumers and manufacturers will be interesting to watch.”
3. Expect manufacturers to make product changes.
When the federal government required that manufacturers add trans fat information on the label a decade ago, the food industry responded by marketing more products with lower trans fats, Crawford said.
“Trans fats are now not allowed to be added to foods during processing, but it all began with labeling,” Crawford said. “We're going to see some big shifts in the marketplace with products lower in sugars such as cereals, yogurts, spaghetti sauces and beverages, of course. We can look forward to recipe reformulation, which will make products more competitive. It's a great first step for reducing sugar consumption. In preparation for the new labels, manufacturers are working on creating products with lower levels of added sugars.”
For manufacturers, the trick will be to keep food tasting good to consumers while reducing sugar, Roberts said. “Other large manufacturers will pursue new products that are not heavy on added sugars,” Roberts said. “For example, Coke and Pepsi sell bottled water.”
“There is a push to at least re-size products,” Schmidt added. “There certainly will be an effort for front-of-package labeling that says ‘low sugar.'”
4. The new label could lead to regulations limiting sugar.
“Including added sugar on the label will be a game-changer for those debates about what is a healthy diet for people in the federal food-assistance programs,” said Schmidt, lead investigator on the UCSF-led SugarScience research and education initiative. “Once you've got added sugar on the label along with a daily reference value, policymakers will be in the position to set standards for the quantity of added sugar allowed in school lunches and other federal food programs.”
Changes like this have happened before, Schmidt noted. “In the U.K., the government said salt consumption is way too high and mandated that packaged food manufacturers reduce the amount of sodium in their products. It worked like a charm – they just gradually reduced the excess salt in foods to everyone's benefit.”
5. The new label makes changes beyond sugar.
The new label also will list more realistic serving sizes and will list calories in a larger and bolder font. “This will help people assess how many calories they are actually consuming,” Swartzberg said. (View a complete list of label changes here.)
6. Further steps could help consumers.
While praising the label changes, UC experts say further steps could help consumers make more informed choices:
- Adding front-of-package labeling that states whether the product is high in sugar, salt or fat: “This banner on the front of packages would make it simple for a consumer to see whether a food is healthy or whether it has ingredients that contribute to risk of heart disease, stroke, obesity or cancer,” Crawford said.
- Having food vendors add “stoplight” stickers: “There is the stoplight idea of labeling products with green, yellow and red stickers – green for the low-sugar products and red for the high-sugar ones,” offered Schmidt.
- Promoting environmentally sustainable food practices: “(We should) consume more plant-based foods and less meat,” Swartzberg suggested.
- Increasing research: “The label change is not enough: Further research, education and sound policies will need to be developed to motivate more healthy eating,” Roberts said.