- Author: Kathy Keatley Garvey

So could research on a fly--a model organism--help us understand and maybe lead to treatment of schizophrenia and other complex disorders?
Postdoctoral fellow Sergio Hidalgo Sotelo of the UC Davis Department will present an in-person seminar on “Using Drosophila melanogaster to Understand Complex Disorders: Insights on the Pathophysiology of Schizophrenia” on Wednesday, Oct. 20 in 122 Briggs Hall, Kleiber Hall Drive.
Sotelo, a researcher in the laboratory of molecular geneticist and physiologist Joanna Chiu, professor and vice chair of the UC Davis Department of Entomology and Nematology, will speak at 4:10 p.m. Plans are to record the seminar for later viewing.
In his abstract, Sotelo relates: “As genome association technologies improve, we have more information regarding the genetic components underlying neurodegenerative and neuropsychiatric disorders such as Alzheimer's, Parkinson's, and schizophrenia. Drosophila melanogaster offers a genetically tractable in vivo system that can be used to perform genetic screens and characterization of genes associated with complex disorders. By combining physiological and behavioral analyses, my work aims to understand the molecular mechanism and neuronal networks involved in some of these conditions.”
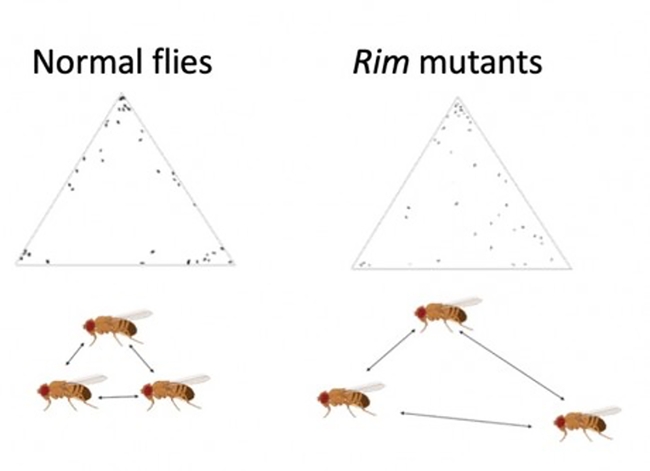
Untangling the Mechanisms. “Schizophrenia is a condition that is characterized by its debilitating and poorly understood symptoms," he pointed out. "By studying the genetic component of this disorder, we aim to untangle the mechanisms behind those symptoms. This could potentially help us to develop new and more effective treatments. Using a similar approach would give us insights better understanding of others disorders like Alzheimer's and Parkinson's.”
Said Professor Chiu: “Sergio's exciting thesis research highlights the value of Drosophila as an animal model to study biological processors. To many, it is probably surprising to hear that this tiny insect is constantly used as an animal model to study complex human diseases such as Alzheimer's and Parkinson's. In fact, there are quite a number of similarities between fly and human physiological systems, even in the brain.”
According to Wikipedia: "Starting with Charles W. Woodworth's proposal of the use of this species as a model organism, D. melanogaster continues to be widely used for biological research in genetics, physiology, microbial pathogenesis, and life history evolution. As of 2017, five Nobel Prizes have been awarded to drosophilists for their work using the animal."
Sotelo joined the Chiu lab as a postdoctoral fellow in the summer of 2020. “Despite the difficult situation brought on by COVID, Sergio is making significant progress in his research on biological rhythms," Chiu said. "He has brought his expertise in neurogenetics, infused the lab with creative energy, and contributed to the training and growth of younger investigators in the lab. Recently, he was named a Pew Latin American Fellow in the Biomedical Sciences, a prestigious award for a well-deserved scientist.”
A native of Puente Alto, Santiago, Chile, Sotelo is one of 10 post-docs from across Latin America—including Argentina, Brazil, Chile, Mexico, Peru, and Uruguay—to receive two years of funding to conduct research. The fellows work under the mentorship of prominent biomedical scientists, including alumni of the Pew Scholars Program in the Biomedical Sciences.
The UC Davis Department of Entomology and Nematology seminars are held on Wednesdays at 4:10 p.m. and include both in-person and virtual lectures. All in-person seminars are held in 122 Briggs Hall, while the virtual seminars are broadcast on Zoom. For more information, contact seminar coordinator Shahid Siddique, at ssiddique@ucdavis.edu.
- Author: Kathy Keatley Garvey

A member of the UC Davis faculty since 1980, Hammock received his doctorate in entomology and toxicology from UC Berkeley, where he studied insect science. He now devotes his research to human health.
What many people do not know, however, is that he began his career studying how caterpillars turn into butterflies.
That morphed into human health research.
“The work led to the discovery that many regulatory molecules are controlled as much by degradation and biosynthesis,” Hammock related. “The epoxy fatty acids control blood pressure, fibrosis, immunity, tissue growth, pain and inflammation to name a few processes.”
Fast forward to today.
An enzyme inhibitor developed in the Hammock lab and tested in mice by a team of international researchers shows promise that it could lead to a drug to prevent or reduce the disabilities associated with the neurodevelopmental disorders of autism and schizophrenia.
What the Inhibitor Did
"We discovered that soluble epoxide hydrolase (sEH) plays a key role in inflammation associated with neurodevelopmental disorders. Inhibiting that enzyme stops the inflammation and the development of autism-like and schizophrenia-like symptoms in animal models,” said collaborator Kenji Hashimoto, a professor with the Chiba University Center for Forensic Mental Health, Japan. The scientists found higher levels of sEH in a key region of the brain—the prefrontal cortex of juvenile offspring-- after maternal immune activation (MIA).

The news embargo lifted today (March 18) on their research, to appear in the Proceedings of the National Academy of Sciences (PNAS). It's the work of 14 researchers from Chiba University Center for Forensic Mental Health; the Laboratory for Molecular Psychiatry, RIKEN Center for Brain Science, in Wako, Saitama, Japan; and the Hammock laboratory.
Reversed Cognitive and Sciatl Interaction Deficiencies
By inhibiting sEH, the researchers reversed cognitive and social interaction deficiencies in the mice pups. They hypothesize that this is due to increasing natural chemicals, which prevent brain inflammation. In people, this could reduce the disabilities associated with autism, such as anxiety, gastrointestinal disturbances and epilepsy.
Earlier studies have indicated a genetic disposition to the disorders. The team also studied postmortem brain samples from autism patients that confirmed the alterations.
“In the case of both autism and schizophrenia, the epidemiology suggests that both genetics and environment are contributing factors,” said neuroscientist and associate professor Amy Ramsey of the Department of Pharmacology and Toxicology, University of Toronto, who was not involved in the study. “In both cases, maternal infection is a risk factor that might tip the scales for a fetus with a genetic vulnerability. This study is important because it shows that their drug can effectively prevent some of the negative outcomes that occur with prenatal infections. While there are many studies that must be done to ensure its safe use in pregnant women, it could mitigate the neurological impacts of infection during pregnancy.”

Neuroscientist Lawrence David, professor and chair of the School of Public Health, University of Albany, N.Y., who was not involved in the research, said that the study might lead to “an important therapeutic intervention for neurodevelopment disorders.”
“There is increasing evidence that maternal immune activation activities (MIA) during fetal development can lead to aberrant neurobehaviors, including autistic-like activities,” said Lawrence, who studies neuroimmunology and immunotoxicology. The study “suggests that enzymatic control of fatty acid metabolism is implicated in neuroinflammation associated with schizophrenia and autism spectrum disorders. The expression of Ephx2 giving rise to soluble epoxide hydrolase (sEH) influences production of fatty acid metabolites, which elevate inflammation in the experimental model of mice after MIA; the sEH inhibitor TPPU (N-[1-(1-oxopropyl)-4-piperidinyl]-N'-[4-(trifluoromethoxy)phenyl)-urea) was postnatally used to improved behaviors. Analysis of cadaver brains from individuals with ASD also expressed increased sEH. Fatty acid metabolites have been known to affect fetal development, especially that of the brain; therefore, TPPU might be an important therapeutic intervention for neurodevelopmental disorders.”
Molecular bioscientist Isaac Pessah of the UC Davis School of Veterinary Medicine, distinguished professor and associate dean of research and graduate education in the Department of Molecular Biosciences, described the findings as “significant” and called for more detailed and expanded studies.

Autism: 1 of 68 Children
The Center for Disease Control and Prevention (CDC) estimates that 1 in 68 children in the United States have autism, commonly diagnosed around age 3. It is four times more common in boys than girls. CDC defines autism spectrum disorder as a “developmental disability that can cause significant social, communication and behavioral challenges.” The disorder impairs the ability to communicate and interact.
Schizophrenia: 1.2 Percent of Population
Approximately 3.5 million people or 1.2 percent of the population in the United States are diagnosed with schizophrenia, one of the leading causes of disability, according to the Schizophrenia and Related Disorders Alliance of America (SARDAA). Scores more go unreported. Approximately three-quarters of persons with schizophrenia develop the illness between 16 and 25 years of age. Statistics also show that between one-third and one half of all homeless adults have schizophrenia, and 50 percent of people diagnosed have received no treatment. Among the symptoms: delusions, hallucinations, disorganized speech, disorganized or catatonic behavior, and obsessive-compulsive disorders, such as hoarding, according to SARDAA.
In their research paper, titled “Key Role of Soluble Epoxide Hydrolase in the Neurodevelopmental Disorders of Offspring After Maternal Immune Activation,” the scientists described sEH as “a promising prophylactic or therapeutic target for neurodevelopmental disorders in offspring after MIA.”
First author Min Ma and second Qian Ren of the Hashimoto lab conducted the animal and biochemical work, while chemists Jun Yang and Sung Hee Hwang of the Hammock lab performed the chemistry and analytical chemistry. Takeo Yoshikawa, a team leader with the RIKEN's Molecular Psychiatry Laboratory, performed measurements of gene expression in the neurospheres from iPSC (induced pluripotent stem cells) from schizophrenia patients and postmortem brain samples from autism patients.
Exciting and Productive
Hashimoto described the international collaboration as “exciting and productive.” This is their third PNAS paper in a series leading to endoplasmic reticulum stress. “We report discovery of a biochemical axis that leads to multiple neurological disorders, including depression, Parkinson's disease, schizophrenia, autism spectrum disorders and similar diseases,” he said.
William Schmidt, vice president of clinical development at EicOsis, a Davis-based company developing inhibitors to sEH to treat unmet medical needs in humans and companion animals, said the company is devel?oping a first-in-class therapy for neuropathic and inflammatory pain. “EicOsis is in the process of finalizing our first human trials on the inhibitors of the soluble epoxide hydrolase, originally reported from UC Davis,” Schmidt said. “We are targeting the compounds as opioid replacements to treat peripheral neuropathic pain. It is exciting that the same compound series may be used to prevent or treat diseases of the central nervous system.”
Several grants from the National Institutes of Health, awarded to Hammock, supported the research. Hammock praised the many collaborators and students he has worked with on the project. “This work illustrates the value of research universities in bringing together the diverse talent needed to address complex problems,” Hammock said. “It also illustrates the value of fundamental science. This autism research can be traced directly to the fundamental question of how caterpillars turn into butterflies.”




