- Author: Kathy Keatley Garvey

A newly published study by a team of scientists at Chiba University, Japan and at the University of California, Davis shows that inhibiting an enzyme, the soluble epoxide hydrolase (sEH), plays a key role in curbing the inflammation associated with the development and progression of Parkinson's disease, an age-related brain disorder that affects a million Americans, mostly 60 and over.
The research, published today in the Proceedings of the National Academy of Sciences, is primarily the work of scientists in the labs of Kenji Hashimoto, a professor with the Division of Clinical Neuroscience, Chiba University Center for Forensic Mental Health, Chiba, Japan, and Bruce Hammock, UC Davis distinguished professor of entomology with a joint appointment in the UC Davis Comprehensive Cancer Center.
“Our research suggests that the sEH inhibitor may prevent the progression of Parkinson's disease (PD) as well as treat patients with dementia of Lewy bodies (DLB) if the sEH inhibitor is used in early phases of patients with these disorders,” said Hashimoto, whose career spans 30 years in the development of blood biomarkers and novel therapeutic drugs and includes more than 550 publications on the topic. “Both PD and DLB are chronic and progressive movement disorders. However, the precise causes of these diseases are largely unknown.”
Statistics indicate physicians diagnose 60,000 new cases of Parkinson's disease every year in the United States. The average age of onset is 60, and is more predominant among men.

Hammock said that the work by lead author Qian Ren and his colleagues in the Hashimoto lab “shows that markers and symptoms of Parkinson's disease in whole mice and in human cells with a mutation associated with Parkinson's disease can be treated with a small druglike molecule. By establishing this causal chain of events leading to Lewy body disorders we can better predict environmental chemicals that could predispose people to Parkinson's disease and possibly even treat the disease.”
The paper, titled “Soluble Epoxide Hydrolase Plays a Key Role in the Pathogenesis of Parkinson's Disease,” is co-authored by 14 scientists, including Professor Hammock and Jun Yang and Sung Hee Hwang, all part of the UC Davis Department of Entomology and Nematology and the UC Davis Comprehensive Cancer Center.
“Although there are many medications available to treat symptoms in PD, these do not prevent the progression of the disease, and, to date, no agent with a disease-modifying or neuroprotective indication for PD has been approved,” said Hashimoto. “Therefore, the development of new drugs possessing disease-modifying and /or neuroprotective properties is critical.”
In research studies involving mice, the scientists found “that sEH plays a key role in the inflammation associated with PD pathogenesis and the mechanisms that lead to the disease,” Hashimoto said. “The sEH inhibitor or deletion of the sEH gene protected against MPTP-induced neurotoxicity in mouse brain.” MPTP is an acronym for methyl-4-phenyl-1, 2, 3, 6 tetrahydropyridine, a relative of cyperquat and paraquat herbicides. “Our findings indicate that sEH inhibitors or epoxy fatty acids mimics may be promising prophylactic or therapeutic drugs for alpha-synuclein-related neurodegenerative disorders.”

Robert Higgins, emeritus professor of neuropathology at the UC Davis School of Veterinary Medicine, said: "I find it exciting that Ren and colleagues illustrate a promising path to a drug to prevent the progression of Parkinson's disease. It is impressive how far this work has come since we collaborated with Shirley Gee and the Hammock laboratory on developing a sheep model of Parkinson's disease in the early 1980s."
Neurosurgeon Cesar Borlongan of Morsani College of Medicine, University of South Florida, who was not involved in the study, praised the findings as advancing “our understanding of how Parkinson's disease evolves.” Describing Parkinson's disease as “a devastating brain disorder that mostly affects the aging population,” he said: “There is no cure, only relief from symptoms which include tremors, muscle rigidity, slurred speech, and freezing of gait.”
“While we know that a certain group of brain cells that produce dopamine are selectively destroyed in Parkinson's patients, what triggers this brain cell death remains poorly understood,” said Borlongan, a distinguished professor and vice chair for Research, Department of Neurosurgery and Brain Repair. “In their paper, the authors observed that a protein called soluble epoxide hydrolase (sEH) may be key to the demise of the brain dopamine cells. In small and large animal models of Parkinson's disease, and further confirmed in a group of PD patients, this protein is highly elevated in specific regions of the brain implicated in dopamine cell death.”
Borlongan pointed out that “Equally compelling evidence demonstrated that using a drug that inhibits sEH can reduce brain inflammation and levels of sEH and effectively lessen PD-associated toxicity in the animal models of the disease. Clinical trials of sEH inhibitors in heart and lung disease have been ongoing over the last decade, and may facilitate the entry of these drugs for PD. These results advance our understanding of how PD may evolve, but also point to its novel treatment.”
Qing Li, a professor in the Department of Molecular Biosciences and Bioengineering, College of Tropical Agriculture and Human Resources, University of Hawaii at Mānoa, who also was not involved in the study, called Parkinson's disease “a devastating neurodegenerative disorder that affects patients and caregivers alike with a significant economic burden in the United States and worldwide.”

This basic research drew support from several grants from Japan, including the Strategic Research Program for Brain Sciences, and at UC Davis, grants funded by the National Institute of Health's Institute of Environmental Health Sciences (NIH/NIEHS), and the NIEHS Superfund Program.
Hammock, a member of the National Academy of Sciences and the National Academy of Inventors, has directed the NIH/NIEH Superfund Program for more than 30 years.
Hammock said the soluble epoxide hydrolase inhibitors that inhibit the soluble epoxide hydrolase will soon enter human clinical trials supported by the NIH-NINDS Blueprint Program (NIH's Health's National Institute of Neurological Disorders and Stroke). “These drugs could provide relief for patients with a wide variety of inflammatory diseases,” he said.
The Hammock laboratory has published nearly 900 peer-reviewed papers on the sEH enzyme, discovered while Hammock and Sarjeet Gill (now of UC Riverside) were researching insect developmental biology and green insecticides at UC Berkeley. The work, begun in 1969, led to the discovery that many regulatory molecules are controlled as much by degradation as by biosynthesis, Hammock said. These epoxy fatty acid chemical mediators control blood pressure, fibrosis, immunity, tissue growth, and pain and inflammation.
To date, journals have published more than 17,000 peer-reviewed papers on the sEH enzyme and its inhibitors. Hammock credits the NIEHS for supporting his research in this area since the 1970s.
A Davis-based company, EicOsis, is developing inhibitors to sEH
to treat unmet medical needs in humans and animals. The company recently received a multi-million dollar grant from the NIH/NINDS Blueprint Program to move sEH inhibitors through phase I human clinical trials. “We are developing a non-opiate analgesic to treat the chronic pain often associated with diabetes,” said William Schmidt, vice president of clinical development at EicOsis. “Once we have investigational new drug status from the Food and Drug Administration and have finished our phase I trial, physicians will be able initiate their own trials with the EicOsis compound on Parkinson's disease and other Lewy body disorders.”

- Author: Kathy Keatley Garvey

“We think that this research will lead to a very positive outcome to improve the lives of cystic fibrosis patients,” said co-author Bruce Hammock, distinguished professor in the UC Davis Department of Entomology and Nematology who holds a joint appointment with the UC Davis Comprehensive Cancer Center.
The research, published in the current edition of the Proceedings of the National Academy of Sciences, links a newly discovered class of bacterial enzymes to battling cystic fibrosis, a progressive, genetic disease characterized by persistent lung infections and inability to breathe normally.
Senior author Jennifer Bomberger of the Department of Microbiology and Molecular Genetics, University of Pittsburgh School of Medicine explained that the opportunistic bacterium, Pseudomonas aeruginosa, outcompetes other microorganisms in a cystic fibrosis patient's lungs and establishes a stronghold.

The scientific discovery could lead to new therapies that would interrupt or correct the bacterial sabotage, Hammock and Bomberger said.
“This paper is the outcome of an exciting and interdisciplinary project,” said Hammock, who directs the UC Davis Superfund Program financed by the National Institutes of Health's National Institute of Environmental Health Sciences (NIH-NIEHS).
“It started several years ago with the NIEHS Superfund Program funding both a group at Dartmouth and at UC Davis. A very productive and exciting collaboration resulted in looking at how to mitigate the effects of environmental chemicals on human health. Our collaborative work led to this joint publication which yields exciting hope for cystic fibrosis patients.”
Bomberger continues to work on the biology of the system while the Dartmouth and Davis groups have developed inhibitors of the action of CIF to stabilize pro-resolving mediators, reduce inflammation, and control periodic flare ups of bacterial infections.
"It will be key to devise a way to remove P. aeruginosa's ability to capitalize on the body's natural inflammatory response, without eliminating that response," said Bomberger. "Inflammation is happening for a reason—to clear infection. We just need it to temper the response when it is not effectively doing its job or is no longer needed."
Other co-authors of the paper include Hammock lab members Christophe Morisseau and Jun Yang, both from the UC Davis Department of Entomology and Nematology and UC Davis Comprehensive Cancer Center. .Institutions involved in the study also included the Harvard School of Medicine.

- Author: Kathy Keatley Garvey

The study suggests that wild bee populations likely declined in areas comprising 23 percent of the nation between 2008 and 2013, a decline associated with conversion of natural wild bee habitat into intensive agriculture.
The paper, titled “Modeling the Status, Trends and Impacts of Wild Bee Abundance in the United States,” is published today (Dec. 21) in the Proceedings of the Natural Academy of Sciences.

The seven-member team, led by Insu Koh of the Gund Institute for Ecological Economics at the University of Vermont, Burlington, integrated a wild bee habitat model, land cover data and expert knowledge to map U.S. bee abundance and trends. Pollination ecologist Neal Williams of UC Davis led efforts to assess habitat quality.
Wild bees and pollination demands
“We see striking mismatches in many places between the demand for pollination and the ability of wild pollinators to support that need,” said Williams, an associate professor in the UC Davis Department of Entomology and Nematology, who helped design the study and led efforts to assess bee habitat quality as part of the Integrated Crop Pollination (ICP) Project (http://icpbees.org/.
“Indeed it is crops where demand has most increased that we estimate greatest decline in wild pollinator supply,” Williams said.
“The research is also unique in including uncertainty in our knowledge of the quality of habitat for pollinators and thus recognizes where more effort is needed to understand the vulnerability of pollination services,” he added.
Williams noted that the paper has the potential to bring wider attention to the correlation between the status of wild bee communities and crop pollination demands nationally.
Mismatch in pollination supply and demand
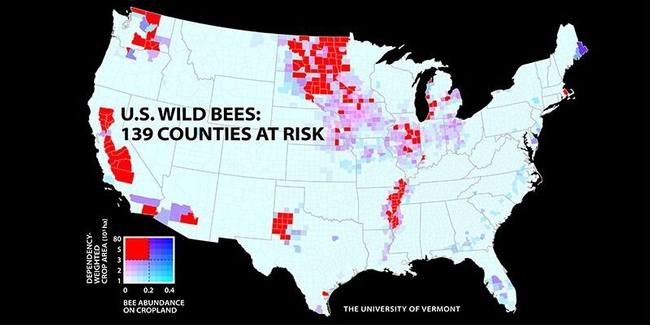
The researchers determined that 139 key counties, comprising 39 percent of U.S. pollinator-dependent crop area, exhibit a “mismatch between pollination supply and demand,” with large areas of pollinator-dependent crops and low expected abundance of wild bees.
The authors noted that the supply of managed honey bees has not kept pace with pollination demand and needs, due to management challenges and colony loss over the last decade. “There is growing evidence that wild, unmanaged bees can provide effective pollination services where sufficient habitat exists to support their populations,” they wrote.
“Until this study, we didn't have a national mapped picture about the status of wild bees and their impacts on pollination,” Koh said. More than $3 billion of the U.S. agricultural economy depends on the pollination services of native pollinators like wild bees.
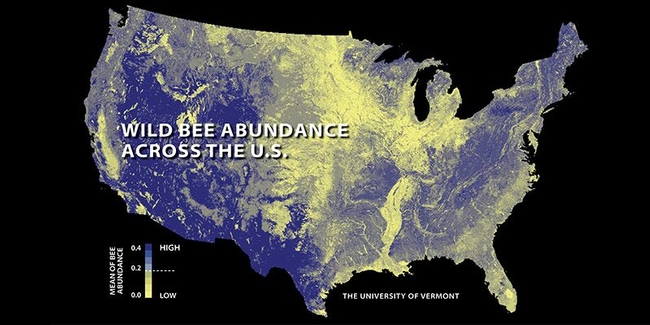
Some of the most important crop pollinators are bumble bees, which have declined over the past decades. “Our mapped index of bee abundance clearly shows that areas of intense agriculture (e.g. the Midwest Corn Belt and California's Central Valley) are among the lowest in predicted wild bee abundance,” the authors pointed out.
Helping agriculture preserve wild pollinators
The authors agreed that the study results may help farmers and agricultural stakeholders develop management efforts to preserve wild bee populations and their pollination services in farmland. Just like honey bees, wild bees are important pollinators and face many of the same threats including habitat loss, environmental pesticide exposure, and climate change.
In addition, the results may help wild bee researchers focus attention on poorly understood regions, the authors said.
Responding to White House call
The study comes on the heels of a 2014 U.S. presidential memorandum calling for a national assessment of pollinators to promote the health of honey bees and other pollinators. One goal is to set aside 7 million acres over a five-year period for pollinators.
Williams said that the modeling study provides important information. “Such assessment is highly valuable in response to calls at the federal level (the White House memorandum and resulting agency responses) to direct research and management efforts to wild pollinators,” he said. “I really hope the paper will generate additional original efforts to improve our understanding of the challenges facing pollinators and their critical role in sustainable food supply.”
Collaborators:
The team also included Claire Brittain of the Neal Williams lab, UC Davis Department of Entomology and Nematology; Taylor Ricketts of the Gund Institute and the University of Vermont; Eric Lonsdorf of Franklin and Marshall College, Lancaster, Pa.; and Rufus Isaacs and Jason Gibbs of Michigan State University, East Lansing.
The study was completed with support from the Specialty Crop Research Initiative of the U.S. Department of Agriculture's National Institute for Food and Agriculture.
Contact:
Neal Williams
nmwilliams@ucdavis.edu
(530)-752-9358
Related Links:
PNAS Online
Online News Release from University Vermont

- Author: Kathy Keatley Garvey


Yes, it can--at least in genetically obese mice, according to a newly published study by researchers in the Joan Clària laboratory at the University of Barcelona, Spain, in collaboration with the Bruce Hammock laboratory of the University of California, Davis. The research involves a potent enzyme inhibitor discovered by the Hammock lab that dramatically reduces inflammation, inflammatory pain and neuropathic pain.
The groundbreaking study, published in the Proceedings of the National Academy of Sciences, involved an enzyme called soluble epoxide hydrolase (sEH) inhibitor used in mice with a high level of omega-3 fats. This treatment both prevented the onset of diabetes and reversed the effects of diabetes in obese mice.
“Our previous studies show the drug we are working on will reduce the symptoms of diabetes in mice by itself,” Hammock said, “but the excitement about Joan Clària's work is that if the mice have a genetically increased level of omega 3 fatty acids --the drug offers prevention or cure in mice.”
Worldwide, 347 million people have diabetes, according to the World Health Organization. The Center for Disease Control and Prevention (CDC) estimates that 29.1 million Americans or 9.3 percent of the population have diabetes, which is characterized by abnormal blood glucose levels. This includes 21 million diagnosed with diabetes, and 8.1 million undiagnosed.
“Epoxide metabolites of the omega 3 fatty acid DHA are stabilized by inhibiting an enzyme soluble epoxide hydrolase or sEH, and these metabolites contribute a great deal to the beneficial effects of an omega-3 diet,” Hammock explained. Previous UC Davis research in the laboratories of Bruce Hammock, Nipavan Chiamvimonvat, Robert Weiss, Anne Knowlton and Fawaz Haj showed that the enzyme reduces or reverses such diabetes-linked medical issues as renal failure, hypertension, diabetic pain, hardening of the arteries, and heart failure.
“This exciting research brings mechanistic detail to understanding how omega-3 fatty acids in the diet exert important health effects,” said UC Davis Professor J. Bruce German, director of the Foods for Health Institute, Department of Food Science and Technology, who was not involved in the diabetes-based research. “Such breakthroughs catalyze both research and practical health applications.”
The Joan Clària lab in Barcelona led the eight-member team study. Clària is an associate professor at the Barcelona University School of Medicine and a senior consultant at the Biochemistry and Molecular Genetics Service of the Hospital Clínic of Barcelona.
In the paper, titled “Inhibition of Soluble Epoxide Hydrolase Modulates Inflammation and Autophagy in Obese Adipose Tissue and Liver: Role for Omega-3 Epoxides,” Clària described the administration of the sEH inhibitor as “a promising strategy to prevent obesity-related co-morbidities.” He said the study “demonstrates that stabilization of cytochrome P-450 epoxides derived from omega-3 polyunsaturated fatty acids through inhibition of the inactivating enzyme soluble epoxide hydrolase (sEH) exerts beneficial actions in counteracting metabolic disorders associated with obesity, including insulin resistance and fatty liver disease.”

In addition to Clària and Hammock, the publication was first-authored by Cristina López-Vicario and co-authored by José Alcaraz-Quiles, Verónica García-Alonso, Bibiana Rius, Aritz Lopategi, Ester Titos and Vicente Arroyo, all of the Clària lab or associates; and Sung Hee Hwang of the Hammock Lab, UC Davis Department of Entomology and Nematology and the UC Davis Comprehensive Cancer Center
Clària's primary research focuses on the study of inflammatory lipid mediators involved in the development of adipose tissue inflammation and its impact on metabolic complications associated with obesity. His laboratory is centered in exploring the role of bioactive lipid mediators generated from omega-3 polyunsaturated fatty acids, especially those with anti-inflammatory and pro-resolution properties. His work places major emphasis on prevailing obesity associated hepatic co-morbidities, especially on non-alcoholic fatty liver disease.
Hammock, who holds a joint appointment with the UC Davis Department of Entomology and Nematology and the UC Davis Comprehensive Cancer Center, has worked on the mechanism of hydrolytic enzymes and their effect on human health for more than 35 years. He is developing both enzyme inhibitors and natural products as drugs for use in the United States and developing countries. His work has helped identify new targets for the action of drugs and other compounds to improve health and predict risk from various environmental chemicals.
Hammock is the founder and CEO of EicOsis, and through EicOsis, the compounds are in clinical trials for companion animals and the Pre-Investigational New Drug Application (Pre-IND) Consultation Program for neuropathic pain in human diabetics.
Hammock was recently selected a fellow of the National Academy of Inventors (NAI), which honors academic invention and encourages translations of inventions to benefit society and a member of the National Academy of Sciences. He directs the campuswide Superfund Research Program and National Institutes of Health Biotechnology Training Program.
The study was funded by Clària's Spanish-initiated grants and by Hammock's Research Project Grant (R01) and Superfund grants from the National Institutes of Health.
Links:
Bruce Hammock lab
http://www.biopestlab.ucdavis.edu/
Email: bdhammock@ucdavis.edu
Joan Clària lab
http://cdb.hospitalclinic.org/facultativos/38/joan-claria-enrich
Email: JCLARIA@clinic.ub.es
PNAS Paper
http://www.pnas.org/content/early/2014/12/30/1422590112.abstract

- Author: Kathy Keatley Garvey
(News embargo lifts at noon Monday, May 19, 2014, Pacific Time)

Listen to Video, Robert Reiner (YouTube, Created by Professor James Carey)
DAVIS--Newly published research involving a 12-year study of dengue infections in Iquitos, Peru—an international team project led by researchers at the University of California, Davis—helps explain why interventions are frequently unsuccessful in efforts to prevent the mosquito-borne disease.
The research, headed by Professor Thomas Scott of the UC Davis Department of Entomology and Nematology, is published May 19 in Proceedings of the National Academy of Sciences (PNAS).
"Defining variation in the risk of dengue transmission has been a roadblock to understanding disease dynamics and designing more realistic and effective disease prevention programs,” said Scott, noted dengue researcher and a senior author of the paper, “Time-Varying, Serotype-Specific Force of Infection of Dengue Virus.”
“This study is an important step toward overcoming that obstacle,” Scott said. “We hope our results will help reduce the burden of this increasingly devastating disease."

“Typically, most infections go unnoticed and as such, measuring and modeling transmission intensity is problematic,” Reiner said.
Dengue virus is transmitted by Aedes aegypti, a mosquito that bites during the daytime as people move about in their daily routines.

“Our work suggests that certain serotypes can infect up to 33 percent of the susceptible population in a single year and that 79 percent of the population of Iquitos would need to be protected from any further infection to eliminate transmission. Further, our estimates form a detailed description of virus transmission dynamics that provides a basis for understanding the long-term persistence of dengue and for improving disease prevention programs.”
Reiner, who holds a doctorate in statistics from the University of Michigan, joined the Scott lab in September 2011. He has just accepted a position as assistant professor in the Department of Epidemiology and Biostatistics, Indiana University, Bloomington.

“The marked variation in transmission intensity that we detected indicates that intervention targets based on one-time estimates of the force of infection (FoI) could underestimate the level of effort needed to prevent disease,” the authors wrote in their abstract. “Our description of dengue virus transmission dynamics is unprecedented in detail, providing a basis for understanding the persistence of this rapidly emerging pathogen and improving disease prevention programs.”

“There is no vaccine nor drug that is effective against this virus,” said Scott, who has studied dengue more than 25 years and is recognized as the leading expert in the ecology and epidemiology of the disease.
While vaccines are under development, it is not clear how they can be best applied when they are available, including in combination with other interventions like mosquito control, Scott said. “New disease prevention tools, in addition to vaccines, and an improved understanding of virus transmission dynamics, which will enhance surveillance and epidemic response, are needed to reduce the global burden of dengue.”
The work was supported by the RAPPID program of the Science and Technology Directory, Department of Homeland Security, and Fogarty International Center, National Institutes of Health; Innovative Vector Control Consortium; U.S. Department of Defense Global Emerging Infections Systems Research Program Work Unit; Military Infectious Disease Research Program Work Units; Deployed Warfighter Protection Program, Department of Defense; and a Wellcome Trust.



