- Author: Kathy Keatley Garvey

Lark Coffey, an assistant professor in the Department of Pathology, Microbiology and Immunology, UC Davis School of Veterinary Medicine and a member of the Center for Vectorborne Diseases, will speak on "Zika Virus in Macaques, Mice and Mosquitoes: Contrasting Virulence and Transmissibility in Disparate Hosts."
And her host is medical entomologist and seminar coordinator Geoffrey Attardo, assistant professor in the UC Davis Department of Entomology and Nematology. This is part of the department's series of fall seminars.
Coffey says on her website: "Mosquito-borne viruses like Zika, chikungunya, West Nile, St. Louis encephalitis and dengue virus are expanding to cause more human infections worldwide. Unfortunately, no licensed human vaccines for these viruses are available. Management of disease is therefore restricted to palliative care for infected people and minimizing exposure to mosquitoes. Our research focuses on several central themes with a common goal of reducing the burden of disease caused by arboviruses. These include: understanding viral genetic factors that promote arbovirus outbreaks predicting viral mutations that enhance arbovirus transmissibility by mosquitoes and disease in humans or animals increasing safety of candidate live-attenuated vaccines improving arbovirus surveillance in mosquitoes."
Her abstract of her seminar Nov. 7 is technical. "Fetal microcephaly and death are now recognized as severe forms of congenital Zika syndrome; however, it is still unclear whether recent Zika virus (ZIKV) mutations contribute to this phenotype," Coffey says in her abstract. "We identified a single intrahost variant in the ZIKV NS2B protein (NS2BM1404I) from a rhesus macaque (RM) fetus that died after experimental ZIKV inoculation in the first trimester. Targeted deep sequencing flanking NS2B1404 in subsequent cohorts of RM mothers and their fetuses identified NS2BM1404I at minority frequency and sometimes at consensus levels in 3 additional dead or stillborn RM fetuses and/or the plasma of their mothers and in 2 more RM mother and fetus pairs whose fetuses survived to near term or were born alive. In outbred pregnant mice inoculated subcutaneously, we observed that NS2BI1404 engineered into an infectious clone confers fetal infection while ZIKV-NS2BM1404 does not. By examining sequence data from recent epidemics, we found that NS2BM1404I occurs rarely (5/500, 1%) in consensus human ZIKV genomes.
"We also deep sequenced ZIKV genomes from non-pregnant human adults, infants, and Ae. aegypti from the epidemic and observed that NS2BI1404 was more often present at intra-host levels in humans compared to mosquitoes," she continues in her abstract. "Since the primary ZIKV transmission cycle is human-mosquito-human, viral mutations that arise in one host must be maintained in the alternate host to be perpetuated. We therefore hypothesized that ZIKV NS2BM1404Imay not be efficiently transmitted by Aedes aegypti mosquitoes, explaining its low frequency in humans during outbreaks. Using infectious clone-derived ZIKV, we examined vector competence in Ae. aegypti from Puerto Rico. Although infection and dissemination rates were not different, we found that Ae. aegypti did not transmit ZIKV-NS2BI1404 as efficiently compared to ZIKV-NS2BM1404 5 [7/20 (35%) versus 10/20 (50%), p>0.05] and 7 [3/20 (15%) versus 13/20 (65%), P<0.001, Chi-squared] days post-feed. The poor transmissibility of this potentially vertebrate adaptive ZIKV mutation may explain its low frequency in febrile humans. This data highlights the evolutionary complexity during arbovirus transmission cycles and suggests that some pathogenic viral mutations are not likely to spread in epidemics."
Coffey received her bachelor of science degree in biology from the University of the South, Sewanee, Tenn., in 2000, and her doctorate in experimental pathology at the University of Texas Medical Branch, Galveston, Texas in 2005.

- Author: Kathy Keatley Garvey

Thanks to the generosity of his family, his work is continuing through memorial research grants to outstanding graduate students at the University of California, Davis.
Hazeltine, a native of San Jose, was a U.S. Navy veteran who studied entomology at UC Berkeley and received his doctorate in entomology from Purdue University in 1962. He managed the Butte County Mosquito Abatement District, Oroville, from 1966 to 1992, and the Lake County Mosquito Abatement District from 1961-1964.
He was an ardent supporter of the judicious use of public health pesticides to protect public health, remembers Bruce Eldridge, emeritus professor of entomology at UC Davis and former director of the (now folded) statewide UC Mosquito Research Program. Eldridge eulogized him at the 2005 annual meeting of the American Mosquito Control Association (AMCA) as "a man who made a difference." The AMCA journal published his eulogy in its 2006 edition. (See http://entomology.ucdavis.edu/files/154217.pdf)
"Bill was a medical entomologist who had a varied career in the field of mosquito biology and control, but he will forever be remembered as a man who fought in the trenches of the pesticide controversy from 1960 until the end of his life, and who made the safe and efficient use of pesticides in public health a personal crusade," Eldridge said.
In his memory, his three sons--Craig Hazeltine of Scottsdale, Ariz., Lee Hazeltine of Lincoln, formerly of Woodland, and the late Jeff Hazeltine (1958-2013)—established the UC Davis Bill Hazeltine Graduate Student Research Awards in 1997. Each year they travel to Davis to honor the recipients at a luncheon, timed with their attendance at a scholarship and fellowship celebration, hosted by Dean Helene Dillard, UC Davis College of Agricultural and Environmental Science.
The 2017 recipients are
- Olivia Winokur of the Christopher Barker lab, Department of Pathology, Microbiology and Immunology, School of Veterinary Medicine. Her funded project ($2425): “Identifying Aedes Mosquito Eggs Using Hyperspectral Imaging: a Rapid, Low-Cost, Non-Destructive Method to Improve Mosquito Surveillance and Control.”
- Maribel "Mimi" Portilla of the Sharon Lawler lab, UC Davis Department of Entomology and Nematology. Her funded project ($2032): “The Management of Invasive Weeds and their Effects on Larval Culex mosquitoes."
Winokur is also the newly announced 2018 recipient of $3,094 to investigate Aedes aegypti immune response to Zika virus. (Portilla expects to receive her doctorate in six to 12 months.)
Olivia Winokur
“Aedes aegypti and Aedes albopictus are mosquitoes capable of transmitting dengue, chikungunya, yellow fever, and Zika viruses,” Olivia Winokur explained in her 2017 application. “These species are invasive and present in California and continue to spread, increasing the likelihood of local transmission of these devastating viruses. Additionally, Aedes notoscriptus, an Australian mosquito whose vector competence for many viruses is unknown, has been detected in Los Angeles and is likely to spread in the state. Aedesmosquitoes are readily detected using ovitraps, a cheap and effective sampling method to detect the presence of gravid females. Ovitraps are especially useful when mosquito populations are low as traps for adult Aedes are unreliable. Once collected, the eggs cannot be differentiated using a stereomicroscope. Traditionally, identifying Aedes eggs collected in ovitraps requires hatching and rearing to adult for visual identification, which is time consuming and leads to a time lag for control, potentially allowing invasive species to spread without intervention.”
“Currently, I am developing a non-destructive, low-cost method to rapidly identify Aedes eggs,” Winokur wrote. “I have shown that species-specific surface morphologies of the exochorion can be used to differentiate species using electron microscopy. This method is expensive and therefore not a realistic surveillance technique. We can, however, exploit these species-specific surface morphologies in another way to identify Aedeseggs. Slight changes in morphological characteristics can be captured with high spatial resolution proximal sensing imaging, termed hyperspectral imaging.”
Winokur is testing “the use of hyperspectral imaging to differentiate between eggs collected from lab colonies of native and invasive Aedes mosquitoes in California. Preliminary data indicate this method shows promise for identifying species and warrants further testing. Once I have created species-specific reflectance profiles and validated my identification method using colony eggs, I will collect field eggs and validate the identification method using these field eggs.” She is working with hyperspectral imaging expert Christian Nansen, agricultural entomologist and assistant professor, UC Davis Department of Entomology and Nematology, on the project.
Winokur describes hyperspectral imaging as “a powerful tool that recognizes slight changes; therefore, we need to ensure that all samples are collected and conditioned the same way before testing. Samples must be imaged directly on the oviposition paper because exochorion cells are damaged by the ‘glue' the female uses to attach her eggs to the substrate; imaging removed eggs leads to inconsistent reflectance profiles. This method for rapidly identifying Aedes eggs will allow for quick response to the detection of invasive Aedes mosquitoes.”
After finishing her Ph.D., Winokur plans to remain in academia, but “I'm unsure exactly what that will look like! I really enjoy research, teaching, and mentoring so I'd like to have a career where I can do all of these. I also plan to have a career where I can conduct translational research with broad global health implications, engage non-scientists, create tools to help decision makers mitigate vector-borne disease burden worldwide, and encourage interest and diversity in STEM (science, technology, engineering and mathematics).”
Maribel "Mimi' Portilla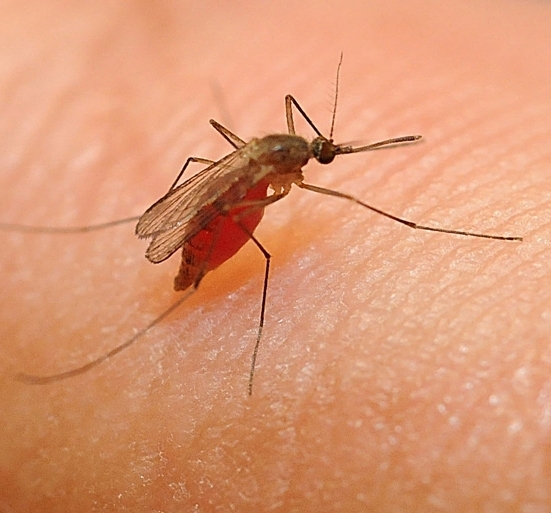
“At UC Berkeley School of Public Health, I was able to study health and disease within a larger context, and learned to consider the biological and the social determinants of disease. As I completed my degree, I realized I really missed the research experiences I had as an undergraduate. So, I looked for a way to bridge my new-found passion for public health and basic science research. This led me to UC Davis, where I learned about One Health and am now pursuing a Ph.D in medical entomology. Medical entomology is a perfect example of a One Health field, where I can seek out how interactions between humans and animals impact health. I am particularly interested in researching how disease risk may change as people manipulate the environment."
Her academic life revolves around writing her dissertation; teaching UC Davis classes (she's taught entomology, general biology and One Health classes); research; and public outreach. Since 2012, she has mentored some 30 undergraduate students on developing and executing their research experiments. She praised the “the diversity of my interns; they each brought such important and unique perspectives to the project.”
What are her career plans?
“Due to my diverse interests and skill set, I am very open about my career choices," Portilla said. "I have extensive teaching experience, and would love to be a professor with both teaching and research opportunities. However, there are many opportunities beyond academia. My research is introducing me to many other ways in which my work and research can help keep people safe and healthy. I hope to develop a strong research skill set while at UC Davis, and find a career path which takes advantage of my diverse abilities and love for One Health and Public Health."
Portilla mentioned pursuing a career as a teacher in a small liberal arts school to teach public health, general biology and global diseases classes, as well as do outreach and research. “I'm more of a scientist than an entomologist,” she said.
She may also pursue a career working in vector-control health education at the county, district or state level. “I'm open at this point,” Portilla said. Overall, she is geared toward improving public health outcomes through healthier environments. “I care about how outcomes affect the larger population,” she said.
Meanwhile, it's good to see that William Emery Hazeltine's passion for medical entomology lives on, and to see UC Davis graduate students benefit, all thanks to the generosity and thoughtfulness of the Hazeltine family. The "family" of 42 recipients since 1997 includes Christopher Barker, Winokur's major professor, who received a Hazeltine research award in 2006.
The complete list of recipients:
- 2018: Olivia Winokur (newly announced)
- 2017: Maribel "Mimi" Portilla and Olivia Winokur
- 2016: Sandy Olkowski, Maribel “Mimi” Portilla and Stephanie Kurniawan
- 2015: Sandy Olkowski, Maribel “Mimi” Portilla and Stephanie Kurniawan
- 2014: Martha Armijos, Elizabeth “Lizzy” Glennon and Rosanna Kwok
- 2013: Jenny Carlson, Elizabeth “Lizzy” Glennon and Sandy Olkowski
- 2012: Jenny Carlson, Kelly Liebman and Sandy Olkowski
- 2011: Brittany Nelms Mills, Kelly Liebman and Jenny Carlson
- 2010: Tara Thiemann and Jenny Carlson
- 2009: Kelly Liebman and Wei Xu
- 2008: Ashley Horton and Tara Thiemann
- 2007: Lisa Reimer and Jacklyn Wong
- 2006: Christopher Barker and Tania Morgan
- 2005: Nicole Mans
- 2004: Sharon Minnick
- 2003: Hannah Burrack
- 2002: Holly Ganz and Andradi Villalobos
- 2001: Laura Goddard and Linda Styer
- 2000: Laura Goddard
- 1999: Linda Boose Styer
- 1998: Larisa Vredevoe
- 1997: John Gimnig

- Author: Kathy Keatley Garvey

Meet Olivia Winokur, an enthusiastic, dedicated and multi-talented medical entomologist whose childhood curiosity about a yellow fever vaccination sparked her interest in 'skeeters.
In her youth, Olivia traveled with her parents and brothers to “off-the-beaten-path” locations. “So I was exposed to vector-borne disease awareness from a young age,” she recalled. “When I was 8 years old, I remember getting the yellow fever vaccination and being curious about why I had to get it for a trip to Southern Africa. I think that was my defining moment when I learned mosquitoes are more than just annoying. Since then, I've slept under many mosquito nets and am no stranger to mosquito bites.”
“I didn't think much about making a career out of those 'skeeters, though. I attended Cornell University as undergraduate, where I studied global public health from multiple perspectives. It wasn't until I became a research assistant in Dr. Laura Harrington's lab that I became fascinated with mosquito biology and decided to pursue a career in medical entomology.”
Winokur, who received her bachelor's degree in 2015 from Cornell University, majoring in Interdisciplinary Studies and focusing on the environmental effects on human health, enrolled in the UC Davis graduate program in 2016 as a Ph.D entomology student with a designated emphasis in the biology of vector-borne diseases.
She studies with major professor and UC Davis alumnus Christopher Barker, associate professor and associate researcher in the Department of Pathology, Microbiology and Immunology, School of Veterinary Medicine, who doubles as a graduate student advisor in the UC Davis Department of Entomology and Nematology.
Earlier this year, Winokur received a three-year National Science Foundation Graduate Research Fellowship. A 2017 Bill Hazeltine Memorial Award also helps fund her research.
Her research at UC Davis mainly involves Aedes aegypti, also known as the yellow fever mosquito. “At present, most of the research done on mosquito-borne virus transmission is done under a very narrow range of conditions that reflect a particular mosquito species' 'optimal' rearing and adult environment,” Winokur said. “I'm interested in how conditions outside of this optimal range at both the larval and adult stages affect mosquito-borne virus transmission. I work mostly with Aedes aegypti, which transmits diseases including dengue, Zika, yellow fever, and chikungunya viruses. Currently my research is focused on Zika virus. I hope to determine how the range of conditions mosquitoes encounter outside of the lab alter their life history traits, such as survival and blood feeding behavior, as well as viral transmission so that we can better understand geographical and seasonal mosquito-borne virus risk and eventually mitigate the risk.”
What fascinates her about mosquitoes? “People are usually wowed when I tell them there are over 3500 species of mosquitoes!” she said. “But don't worry.. not all of them transmit human pathogens. I love telling people about the natural history of different genera and species and how this affects the likelihood of pathogen transmission to humans. I'm continually fascinated by how resilient mosquitoes are, how successful they've been throughout history, and how they've completely altered human history. I actually gave a lecture on how vector-borne diseases have altered human history last quarter (Winter 2018) to an undergraduate class led by UC Davis entomology graduate students (Ent10: Natural History of Insects).”
Born in Long Beach, Calif., Olivia grew up in Laguna Niguel, Calif., where she focused on science as a part of the Dana Hills High School Health and Medical Occupations Academy. Olivia also played basketball at Dana Hills and helped the team win its first league title.
What drew her to UC Davis? “I grew up in California so I was familiar with UC Davis from a young age. I actually applied to UC Davis as an undergraduate, but decided to try life on the East Coast instead and attended Cornell University. While at Cornell, I learned a lot about UC Davis as most of my professors had spent some time at UC Davis during their academic tenure, and a lot of the research I was reading was coming out of UC Davis. I was excited to come back to the West Coast for graduate school so UC Davis seemed like an obvious choice!”

Winokur is a co-author of “The Impact of Temperature and Body-Size on Flight Tone Variation in the Mosquito Vector Aedes aegypti (Diptera: Culicidae): Implications for Acoustic Lures," published in April 2017, in the Journal of Medical Entomology. Several other manuscripts are accepted or in preparation.
She has given presentations at the Mosquito and Vector Control Association of California and the American Society of Tropical Medicine and Hygiene.
Dedicated to helping high school girls transition into STEM (Science, Technology, Engineering and Math) careers, Winokur is a founding board member and publicity co-chair of GOALS (Girls' Outdoor Adventure in Leadership and Science). The organization seeks “to cultivate and embolden the next generation of STEM leaders through a free, immersive, field-based summer science program for high school girls.”
“GOALS is for high school girls, inclusive of cis, trans, and gender nonbinary youth who identify with girlhood, to learn science hands-on while backpacking through the wilderness,” Winokur related. “I have worked with an incredible team of UC Davis affiliates to create GOALS to increase opportunities for high school students who identify with girlhood from backgrounds traditionally underrepresented in STEM. Our first trip is happening this summer!” This year's program takes place July 21 to Aug. 5.
Winokur is also a part of the Letters to a Pre-Scientist program “so I get to be a pen-pal to an elementary school student to talk about science!” In addition, she serves as the treasurer of the UC Davis Entomology Graduate Student Association.
Delighted to return to California after being on the East Coast, Winokur spends her leisure time outdoors hiking and backpacking “and exploring the beautiful places near Davis like the Lake Tahoe area and Yosemite. I taught backpacking and wilderness survival skills for Cornell Outdoor Education during college. Additionally, I'm a trivia nerd so I watch a lot of Jeopardy! and play pub trivia with my entomology colleagues weekly. I also enjoy drawing, reading, playing board games, and doing jigsaw puzzles. When I get the chance I enjoy traveling as well--I just returned from Belize and I'll be in Denmark in July!”
After finishing her Ph.D., Winokur plans to remain in academia, but “I'm unsure exactly what that will look like! I really enjoy research, teaching, and mentoring so I'd like to have a career where I can do all of these. I also plan to have a career where I can conduct translational research with broad global health implications, engage non-scientists, create tools to help decision makers mitigate vector-borne disease burden worldwide, and encourage interest and diversity in STEM.”



- Author: Kathy Keatley Garvey

Travelers know Iquitos as the "capital of the Peruvian Amazon" but scientists know it as a hot spot for dengue, a mosquito-borne viral disease with raging outbreaks in many tropical and subtropical countries.
Amy Morrison, stationed in Iquitos full-time, has directed dengue research activities there for the past 15 years. An epidemiologist who joined the UC Davis laboratory of medical entomologist Thomas Scott (now professor emeritus) in 1996, she's a project scientist and scientific director of the Naval Medical Research Unit No. 6 (NAMRU-6) Iquitos Laboratory.
Morrison is back in the states to present a UC Davis seminar on "Targeting Aedes Aegypti Adults for Dengue Control: Infection Experiments and Vector Control in Iquitos" from 4:10 to 5 p.m., Wednesday, Jan. 10, in 122 Briggs Hall, Kleiber Hall Drive.
Hosted by the UC Davis Department of Entomology and Nematology, it's the first in a series of winter seminars coordinated by assistant professor Rachel Vannette and Ph.D student Brendon Boudinot of the Phil Ward lab.
Dengue is a threat to global health, says Morrison, who holds a doctorate in epidemiology from Yale University and a master's degree in public health from UCLA. According to the World Health Organization (WHO), the incidence of dengue has increased 30-fold over the last 50 years and almost half of the world population is now at risk. It's ranked as "the most critical mosquito-borne viral disease in the world."

"Each year, an estimated 390 million dengue infections occur around the world," according to the World Mosquito Program. "Of these, 500,000 cases develop into dengue hemorrhagic fever, a more severe form of the disease, which results in up to 25,000 deaths annually worldwide."
Of the dengue project in Iquitos, Morrison says: "Comprehensive, longitudinal field studies that monitor both disease and vector populations for dengue viruses have been carried out since 1999 in Iquitos. In addition, to five large scale-vector control intervention trials, ongoing data collection has allowed the evaluation of Ministry of Health emergency vector control using indoor ULV space sprays with pyrethroids in concert with larviciding through multiple campaigns, as well as characterize local DENV (dengue virus) transmission dynamics through two and one novel DENV serotype and strain invasions into the city."
"Our research group has also been conducting contact cluster investigations on DENV-infected and febrile control individuals since 2008," Morrison relates. "These studies demonstrated that attack rates were consistent between houses where cases were first detected and recently visited contact houses independent of distance between these locations. Furthermore, contact cluster investigations allow us to identify viremic individuals across the spectrum of disease outcomes including inapparent infections."
"Using DENV positive individuals captured through these and other febrile surveillance protocols, we exposed laboratory reared (F2) Aedes aegypti mosquitoes directly on their arms or legs, and obtained blood samples with and without EDTA for exposure of mosquitoes in an artificial membrane feeder. After a 58-participant pilot study comparing feeding methods, we initiated a direct feeding protocol exposing participants (78 feeds in 31 participants to date). Feeding, survival, midgut infection and systemic dissemination are all higher using direct feeding than indirect feeding methods. Of 22 participants without detectable fluorescent focus assay titers in their serum at the time they were exposed to mosquitoes, 14 infected mosquitoes by at least one method."
"Although virus titer was a predictor of mosquito infection, mosquitoes became infected at low or undetectable titers and with subjects experiencing mild disease. We have evaluated insecticide-treated curtains and a novel lethal ovitrap (Attractive Lethal OviTrap = ALOT) for dengue control. Only the ALOT traps showed a significant impact on dengue incidence corresponding to a modest decrease in vector densities and a shift of the mosquito population age structure in the trap area to younger mosquitoes. Recent evaluations of indoor ULV interventions with pyrethroids suggest that ULV campaigns that reduce Aedes aegypti for at least 3 weeks through multiple fumigation cycles can mitigate DENV transmission during the same season."
Bottom line: "We argue that Aedes aegypti control should focus on interrupting transmission rather than long-term suppression at operationally unachievable levels and that emergency control should be applied at area-wide scales rather than reacting to individual DENV cases."


- Author: Kathy Keatley Garvey

Chemical ecologist and mosquito researcher Walter Leal, distinguished professor in the UC Davis Department of Molecular and Cellular Biology, and his lab collaborated with scientists in Recife to ask “Does Zika Virus Infection Affect Mosquito Response to Repellents?”
The work, funded by the National Institutes of Health, was published Feb. 16 in Scientific Reports of the journal Nature. The researchers used mosquitoes originating from colonies reared by UC Davis medical entomologist Anthony Cornel and from colonies in Recife.
“We used assays mimicking the human arm to test the mosquitoes infected with the Zika virus,” Leal said, “and we asked whether the Zika infection affects mosquito response to repellents.” They tested DEET and Picaridin, considered the top two mosquito repellents. “We discovered that DEET works better than Picaridin against the southern house mosquito, Culex quinquefasciatus, and the yellow fever mosquito, Aedes aegypti, whether infected or not.”
The researchers also found that old mosquitoes that already had a blood meal “were less sensitive to repellents,” said Leal, adding “It was not clear whether this was due to the virus, but mostly likely because of age. ”
“Lower doses--normally used in commercial products--work well for young mosquitoes,” Leal said, “but the old ones are the dangerous ones because they may have had a blood meal infected with virus and there was enough time for the virus to replicate in the mosquito body.”
“The bottom line: to prevent bites of infected mosquitoes, higher doses of repellent are needed. The data suggest that 30 percent DEET should be used. Lower doses may repel nuisance young mosquitoes, but not the dangerous, infected, old females.”
Leal, a native of Brazil, collaborates with Rosangela Barbosa and Constancia Ayres of the Oswaldo Cruz Foundation (FIOCRUZ-PE), Recife, Brazil. The work with infected mosquitoes was conducted at FIOCRUZ-PE.
Leal, Barbosa and Ayres co-authored the paper with Fangfang Zeng and Kaiming Tan, both of the Leal lab; and Rosângela M. R. Barbosa, Gabriel B. Faierstein, Marcelo H. S. Paiva, Duschinka R. D. Guedes, and Mônica M. Crespo, all of Brazil.
The World Health Organization (WHO) recommends that people traveling to or living in areas with Zika virus (ZIKV) outbreaks or epidemics adopt preventive measures, including the use of insect repellents, to reduce or eliminate mosquito bites. Prior to the Feb. 16 published research, it was not known whether the most widely repellents are effective against ZIKV-infected mosquitoes, “in part because of the ethical concerns related to exposing a human subject's arm to infected mosquitoes in the standard arm-in-cage assay,” the researchers pointed out.
They used a previously developed, human subject-free behavioral assay, which mimics a human subject to evaluate the top two recommended insect repellents.
Scientists isolated the Zika virus (ZIKV) nearly seven decades ago from a sentinel rhesus monkey while they were trying to unravel the cycle of sylvan yellow fever virus in Uganda..
According to the Centers for Disease Control and Prevention:
- Zika is spread mostly by the bite of an infected Aedes species mosquito (Ae. aegypti and Ae. albopictus). These mosquitoes bite during the day and night. The virus can also be sexually transmitted.
- Zika can be passed from a pregnant woman to her fetus. Infection during pregnancy can cause certain birth defects.
- There is no vaccine or medicine for Zika.
- Local mosquito-borne Zika virus transmission has been reported in the continental United States.




